Involutional ectropion
Options for surgical management of ectropion
Involutional ectropion
Options for surgical management of ectropion
INITIAL PRESENTATION
Chief Complaint: Epiphora of the left eye
History of Present Illness
A 72-year-old male presents with epiphora of the left eye. This has been present for one year, but has worsened over the last month. He also describes a foreign body sensation in both eyes as well as redness along the left lower eyelid. He denies any history of trauma, skin cancer, surgery, use of topical medications, or significant sun exposure.
Past Ocular History
- Cataracts both eyes (OU)
- Non-exudative age-related macular degeneration OU
Past Medical History
- Hypertension
- Coronary artery disease
Medications
Allergies
Family History
Social History
- No smoking
- No alcohol use
Review of Systems
OCULAR EXAMINATION
Visual Acuity with correction (Snellen)
- Right eye (OD): 20/25
- Left eye (OS): 20/20
Ocular Motility
Intraocular Pressure
- OD: 14 mm Hg
- OS: 11 mm Hg
Pupils
- OD: 5mm (dark) → 3mm (light) with no relative afferent pupillary defect (RAPD)
- OS: 5mm (dark) → 3mm (light) with no RAPD
Confrontation Visual Fields
- Full to counting fingers OU
Slit Lamp Exam
- OD
- Eyelid: Meibomian gland dysfunction, poor snap back test/lower eyelid laxity
- Conjunctiva: No injection
- Cornea: Clear
- Anterior chamber: Deep and quiet
- Iris: Normal architecture, sectoral iris nevus
- Lens: Posterior chamber intraocular lens
- OS
- Eyelid: Meibomian gland dysfunction, poor snap back test/lower eyelid laxity, ectropion, 2.5mm inferior scleral show. [Figures 1 and 2]
- Conjunctiva: White line seen in the inferior fornix
- Cornea: Clear
- Anterior chamber: Deep and quiet
- Iris: Normal architecture
- Lens: 2+ nuclear sclerosis
Dilated Fundus Examination (DFE)
- OD: 0.4 cup/disc ratio, peripheral drusen
- OS: 0.3 cup/disc ratio, peripheral drusen
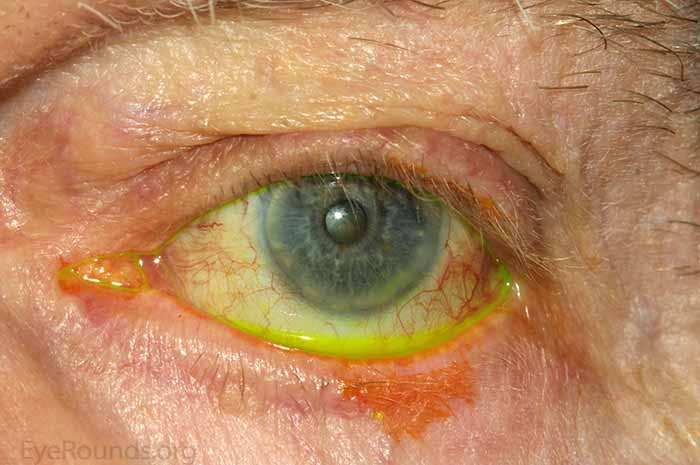
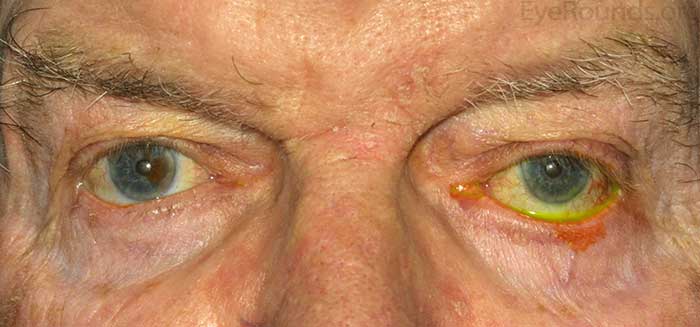
Figures 1 (top) and 2 (bottom): Lower lid laxity with more inferior scleral show on the left compared to the right eye.
Diagnosis: Involutional ectropion
CLINICAL COURSE
The patient underwent ectropion repair with a lateral tarsal strip (LTS) and inverting sutures. Figure 3 shows the post-operative appearance 7 years after the procedure was performed, which illustrates continued stability of the lower lid.
DISCUSSION
Ectropion is one of the most commonly encountered eyelid disorders seen in ophthalmology. It is classified into several different categories including involutional, cicatricial, paralytic, mechanical, and congenital. The most common entity causing this disorder is involutional ectropion. Patients with this disorder frequently experience symptoms of ocular irritation including redness, discharge, papillary conjunctival reaction and corneal epitheliopathy. Exposure of the palpebral conjunctiva causes conjunctival inflammation and poor lower lid protraction may result in inferior corneal exposure. Findings on examination which support the diagnosis of involutional ectropion include poor apposition of the eyelid to the globe, poor snap back test (inability of the eyelid to return to its normal position apposed to the globe after being manually pulled away), positive distraction test (ability to pull eyelid >6mm from the globe), and outward turned lashes. Involutional ectropion should be considered a diagnosis of exclusion in the sense that there should be no anterior lamellar shortening, mechanical cause, or orbicularis weakness to explain the exam findings. One should look closely for these other potential causes of ectropion prior to performing surgical repair.
The most common anatomic changes leading to involutional ectropion are horizontal eyelid laxity, lamellar dissociation, and retractor disinsertion. Other entities such as a large tarsus, relative proptosis, and maxillary hypoplasia may play a role as well. Findings which suggest retractor disinsertion include a white line in the inferior fornix below the tarsus, a deep inferior fornix, and little to no movement of the lower eyelid on downgaze.
Understanding eyelid anatomy is helpful when planning surgical repair. The eyelid is separated into the anterior, middle, and posterior lamella. Superior to the inferior border of the tarsus, the anterior lamella consists of the skin and orbicularis muscle and the posterior lamella consists of the conjunctiva and tarsus. Inferior to the inferior border of the tarsus, the anterior lamella continues as the skin and orbicularis muscle and the posterior lamella continues as the conjunctiva. The middle lamella in this region consists of the lower eyelid retractors, lower eyelid fat pads, and orbital septum. There are multiple surgical options when it comes to repair of involutional ectropion. The severity of ectropion determines which procedure or combination of procedures should be employed. The main goals of repair are focused on tightening of the lower eyelid followed by reassociation of the lamella into their normal anatomic position.
- The primary modality for repair is the lateral tarsal strip which is the most direct way to address horizontal eyelid laxity (2). This procedure can be performed in conjunction with the procedures described below. A horizontally tight lower eyelid is a stable eyelid; therefore, the reinsertion of the strip at the level of Whitnall's tubercle is essential. This results in reattaching the lateral canthal tendon in a relatively superior (classically described as 2 mm superior to the medial canthus) and posterior position. Depending on the axial position of the globe, one might reattach the tendon slightly above (in the case of relative proptosis) or below (in the case of relative enophthalmos) this level.
- For mild cases and cases with punctal malposition, a medial spindle can be used (3). This works well for punctal malposition, but less well for greater degrees of ectropion. In general, this should be considered a relatively weak procedure.
- Retractor reinsertion (transconjunctival or anterior lamella approach) is an effective way to correct instability of the tarsus (4, 5). A risk with this procedure is retraction of the lower eyelid and not adequately addressing lamellar dissociation.
- Inverting sutures can also be used to correct malposition as well by correcting lamellar dissociation.
It is well understood that using a combination of these procedures, when indicated, is a fantastic way to achieve excellent functional and aesthetic outcomes. As noted above, a lateral tarsal strip will almost always be performed in conjunction with a medial spindle, retractor reinsertion, or inverting sutures (in order of increasing severity of the ectropion) (6).
Cicatricial ectropion is usually associated with shortening of the anterior lamellae. It can be caused by prior surgical resections of tissue, burns (thermal or chemical), actinic damage, autoimmune disease, or chronic inflammation (rosacea, dermatitis). Treatment is centered on release of cicatricial changes, followed by horizontal tightening, and then repair of the shortened anterior lamella (skin grafts, midface/cheek lift). A periosteal strip can be used as well to provide more firmly anchored lid in tough cases (7). The midface/cheek lift can be performed with a dissection in the pre periosteal space and suture fixation to the periosteum or subperiosteal plane with the use of a fixating device (endotine midface B) or drilling holes in the inferior orbital rim and suture fixating for more severe cases.
Mechanical ectropion refers to a situation in which a mass on the lower lid is pulling it down/away from the globe. This is usually a pretty obvious diagnosis and treatment is based on removing the mass.
Although lower lid malposition associated with facial paralysis has been classically described as an ectropion, many surgeons now recognize this malposition as a retraction due to the unopposed action of the lower lid retractors. In this situation, horizontal tightening with a lateral tarsal strip combined with recession of the lower lid retractors and placement of a spacer corrects the malposition. For more information regarding eyelid malposition in the setting of a facial nerve palsy, please see this associated case and discussion.
Congenital ectropion is a rare condition usually affecting the upper eyelid. Placement of fornix sutures usually corrects the condition.
Below are instructional videos by Dr. Richard Allen demonstrating how these procedures are performed along with written, step-by-step instructions.
If video fails to load, use this link:
https://vimeo.com/123354779
- A lateral canthotomy is performed with either the needle tip cautery or a #15 blade.
- An inferior cantholysis is then performed with either the needle tip cautery or scissors.
- Dissection is then carried out between the anterior and posterior lamella for approximately 5 to 10 mm, depending on the laxity of the eyelid.
- The mucocutaneous junction is then excised along the length of the strip with Westcott scissors.
- The posterior surface of the strip is then scraped with a 15 blade to denude the area of any epithelium.
- The strip is then grasped and placed into position along the lateral orbital rim to determine the appropriate amount to shorten it, which is performed with Westcott scissors.
- This is usually somewhere around 3-5 mm, depending on the laxity of the lid.
- A double arm 4-0 Mersilene suture on an S-2 needle is then placed so that each arm exits the anterior surface of the strip.
- The needle then engages the lateral orbital rim at the level of Whitnall's tubercle which is at least 2 mm superior to the medial canthus.
- This is placed in the periosteum posterior to the lateral orbital rim.
- The periosteal bite is confirmed by pulling on the sutures.
- The second needle is placed in the same manner. Again, the needle used here is a half circle needle which works well in small spaces.
- The sutures are then tied.
- The canthus is then reformed by excising the lash follicles corresponding to the anterior lamella of the strip.
- The anterior lamella is sutured to the strip medial to the lateral orbital rim with a single 5-0 fast-absorbing sutures.
- The remaining sutures are placed lateral to the lateral orbital rim to repair the canthotomy.
If video fails to load, use this link: https://vimeo.com/123339484
Start this procedure with the LTS, but wait to tie sutures to the lateral orbital rim until the medial spindle is performed.
- Attention is then directed medially where a Bowman probe is placed through the lower punctum and canaliculus.
- Westcott scissors are then used to excise a spindle shaped piece of conjunctiva and lower lid retractors inferior to the inferior boarder of the tarsus straddling the punctum.
- A double armed 5-0 chromic suture is then used to engage the lower lid retractors followed by the inferior boarder of the tarsus. Each arm is placed identically.
- The suture is then placed through the eyelid, entering at the inferior edge of the conjunctival incision and exiting inferonasally through the skin.
- The further inferior you exit the suture, the greater the amount of inversion you will get.
- The lateral tarsal strip sutures are then tied.
- The redundant anterior lamella with lash follicles are excised.
- The canthotomy is then repaired with a 5-0 fast absorbing suture.
- The medial spindle sutures are then tied to invert the medial eyelid margin. Realistically it is very difficult to overcorrect this procedure.
- At the conclusion of the case, the lid is in good position and antibiotic ointment is placed into the eye and the patient returns in one week.
If video fails to load, use this link: https://vimeo.com/123337650
The different steps using the transconjunctival approach are listed here.
- A lateral canthotomy is performed with the #15 blade.
- The monopolar cautery is then used to perform the inferior cantholysis.
- 4-0 silk sutures are then placed through the eyelid margin at the level of the meibomian glands to provide traction during the case.
- The monopolar cautery is then used to make an incision through the conjunctiva and lower lid retractors inferior to the inferior boarder of the tarsus, extending from the lateral canthus laterally to the punctum medially.
- Dissection is then performed in the plane between the lower lid retractors and lower lid fat.
- Westcott scissors are then used to excise approximately 2 to 3 mm of conjunctiva and lower lid retractors. Hemostasis is attained with the monopolar cautery.
- The edge of the conjunctiva and lower lid retractors are then sutured to the inferior border of the tarsus with a running 7-0 vicryl suture, effectively shortening the conjunctiva and lower lid retractors.
- The next step is the lateral tarsal strip.
If video fails to load, use this link: https://vimeo.com/132969584/.
- A lateral canthotomy and inferior canthoysis are performed with the needle tip cautery. A transconjunctival incision is then performed with the needle tip cautery extending from the punctum medially to the lateral canthotomy incision laterally just inferior to the inferior border of the tarsus.
- Dissection is then carried out between the orbicularis muscle and orbital septum to the inferior orbital rim. Using a 5-0 vicryl suture, inverting sutures are placed.
- The suture is placed transcutaneous approximately 1 cm inferior to the inferior border of the tarsus to exit out the orbicularis muscle. The suture then engages the inferior border of the tarsus. The suture is then placed transcutaneously back through the orbicularis and skin to exit adjacent to the entry site.
- An additional suture is then placed centrally and then laterally in the same fashion.
- These sutures are left untied until the end of the case.
- The transconjunctival incision is then closed with interrupted or running 7-0 vicryl sutures. In this case the sutures are placed in an interrupted fashion.
- Next the lateral tarsal strip is performed as previously described.
Summary
These videos and descriptions of surgical technique are created to help surgeons understand repair of ectropion. As a surgeon, one has many options for repair of involutional ectropion. Careful selection of the combination of procedures is key for excellent functional and aesthetic outcomes.
EPIDEMIOLOGY
- One of the most common oculoplastic disorders of the eyelids
|
SIGNS
- Poor snap back test
- Poor distraction test
- Retractor disinsertion
|
SYMPTOMS
- Conjunctival irritation
- Corneal epitheliopathy
- Epiphora
|
TREATMENT
- Lateral tarsal strip
- Medial spindle
- Inverting sutures
- Retractor reinsertion
|
References
- Frueh BR, Schoengarth LD. Evaluation and treatment of the patient with ectropion. Ophthalmology 1982;89:1049–54.
- Jordan DR, Anderson RL. The lateral tarsal strip revisited. The enhanced tarsal strip. Arch Ophthalmol. 1989;107 (4):604-606.
- Nowinski TS, Anderson RL. The medial spindle procedure for involutional medial ectropion. Arch Ophthalmol. 1985; 103(10):1750-1753
- Putterman AM. Ectropion of the lower eyelid secondary to Muller's muscle-capsulopalpebral fascia detachment. Am J Ophthalmol. 1978;85:814-817.
- Tse DR, Kronish JW, Buus D. Surgical correction of lower-eyelid tarsal ectropion by reinsertion of the retractors. Arch ophthalmol. 1991;109(3):427-431
- Ghafouri RH1, Allard FD, Migliori ME, Freitag SK. Lower eyelid involutional ectropion repair with lateral tarsal strip and internal retractor reattachment with full-thickness eyelid sutures. Ophthal Plast Reconstr Surg. 2014 Sep-Oct;30(5):424-6.
- Weinstein GS, Anderson RL, Tse DT, Kersten RC. The use of a periosteal strip for eyelid reconstruction. Arch Ophthalmol. 1985 Mar;103(3):357-9.
Suggested citation format:
Lenci LT, Clark TJ, Allen RC. Involutional ectropion: Options for surgical management of ectropion. EyeRounds.org. posted August 24, 2015; Available from: http://www.EyeRounds.org/cases/218-ectropion.htm
last updated: 08/14/2015
Image Permissions:

Ophthalmic Atlas Images by EyeRounds.org, The University of Iowa are licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License.


