This guide is intended to provide education about eye removal to patients and families who are considering or undergoing eye removal surgery. For many, the idea of removing an eye can be understandably very daunting. However, it is important to know that eye removal is a relatively common surgery that can treat certain eye diseases, alleviate eye pain, and greatly improve the patient's quality of life. It is our hope that this guide will help patients and their families better understand the different procedures used to remove the eye, how to best prepare for the surgery, and what to expect during the healing process.
Figure 1. A typical timeline of events portraying what will happen before, on the day of, and after the eye removal surgery.
There are a variety of reasons that an eye may be removed. Some of the most common indications include trauma, cancer (such as retinoblastoma or ocular melanoma), end stage eye disease (such as diabetic retinopathy, glaucoma, or after multiple eye surgeries), or an otherwise degenerated blind and/or painful eye.
There are two methods to remove an eye: evisceration or enucleation (Figure 2 and Figure 8).
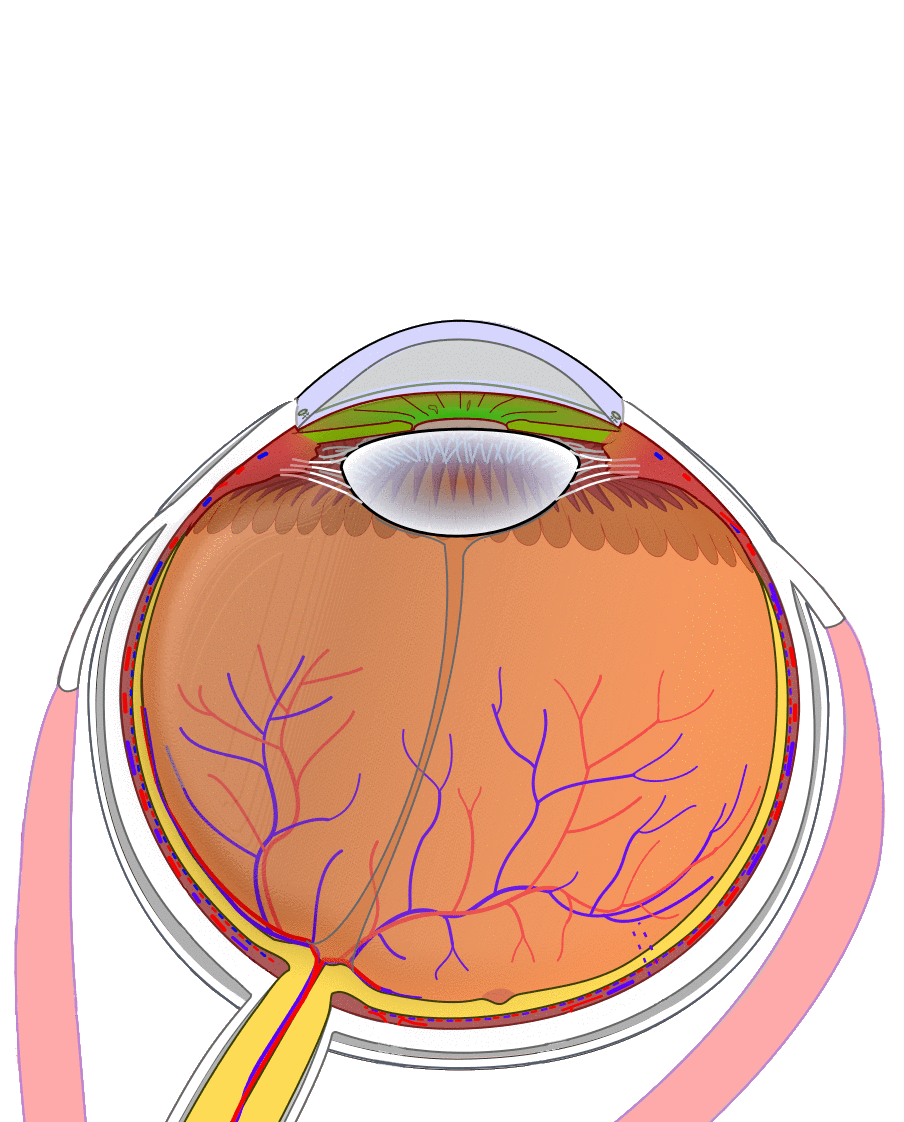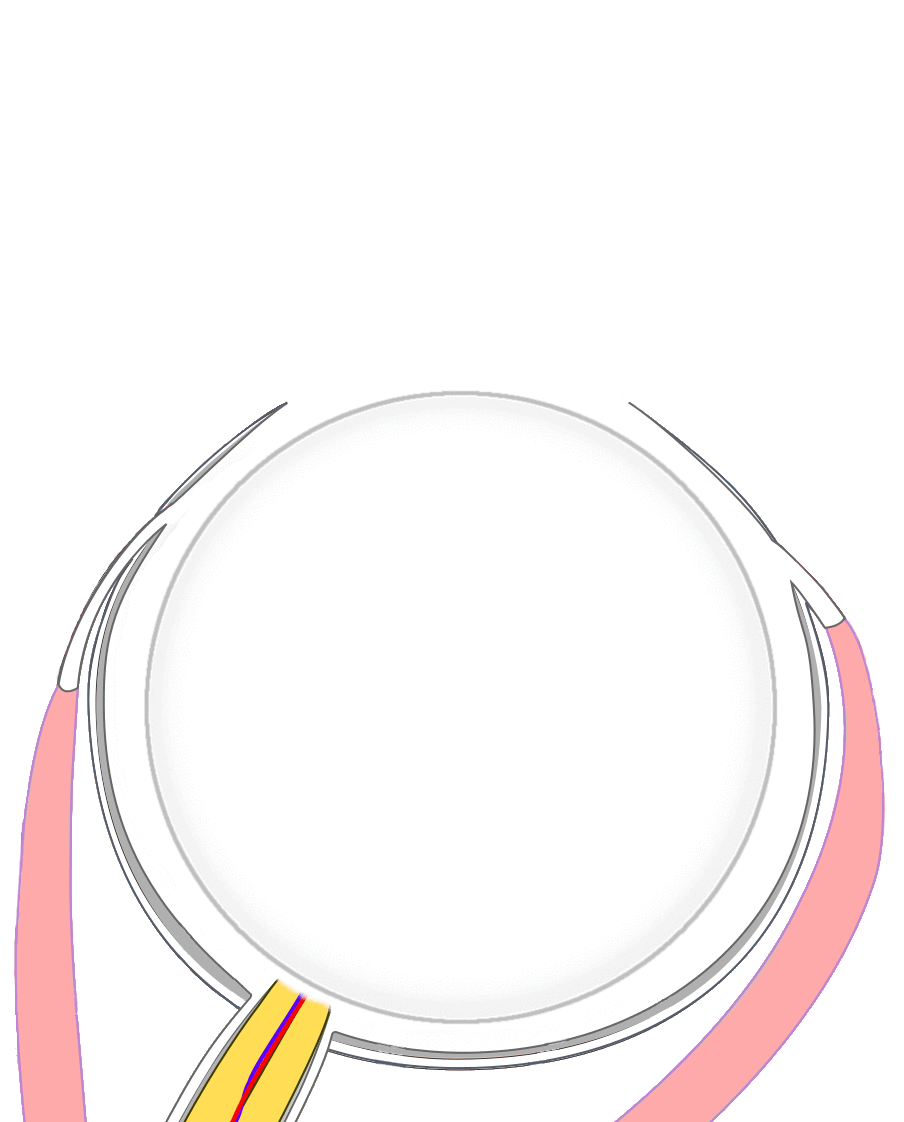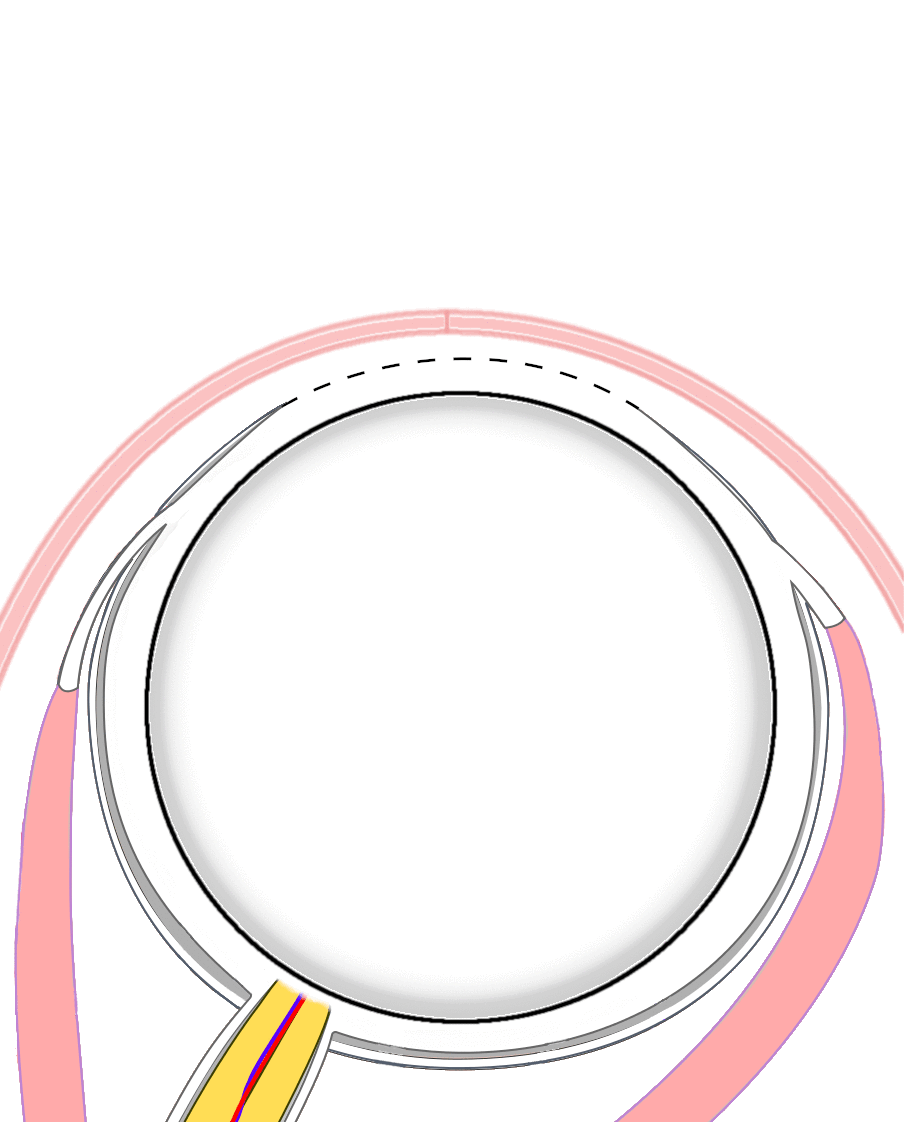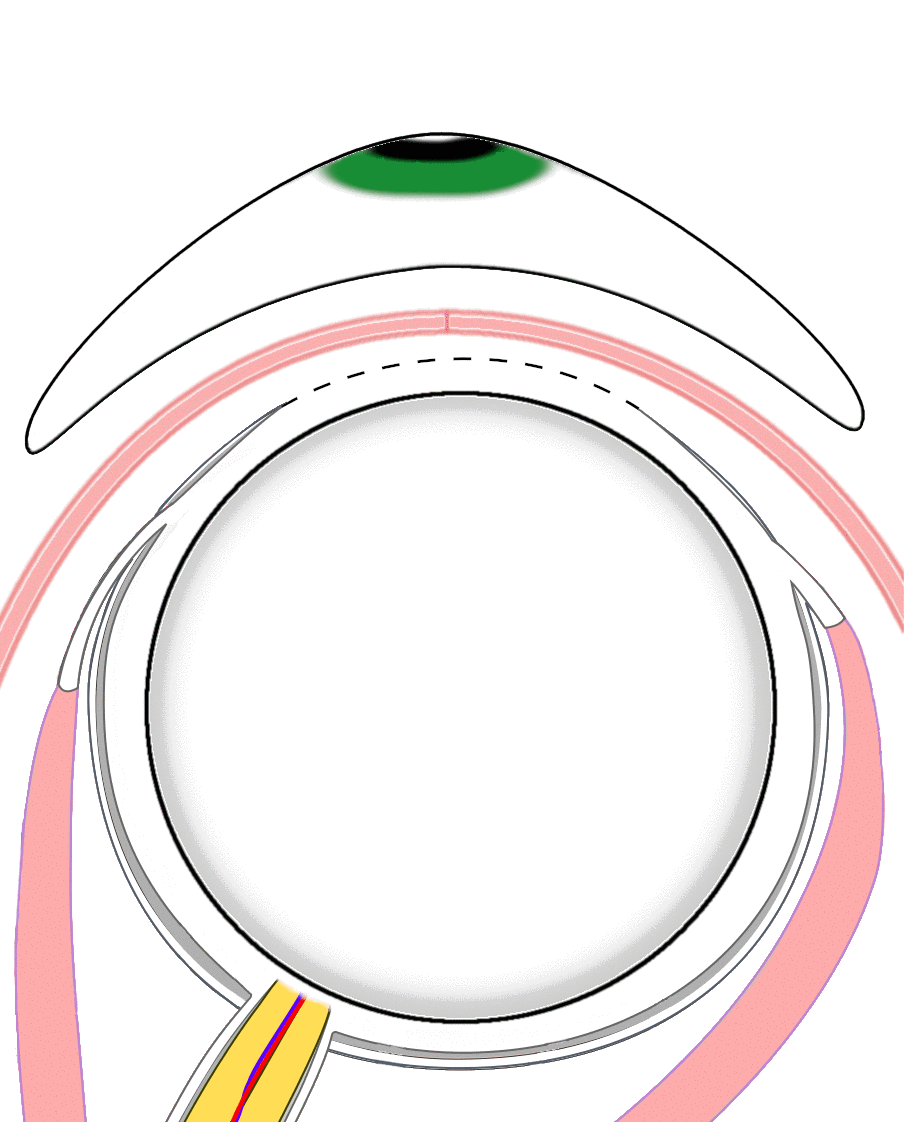
Figure 2a. This graphic highlights the tissues removed during an evisceration. An evisceration removes the intraocular contents (light blue) while preserving the remaining scleral shell, extraocular muscle attachments, and surrounding orbital tissues. |
Figure 2b. This graphic highlights the tissues removed during an enucleation. In contrast, an enucleation detaches the extraocular muscles and removes the entire eyeball – both the intraocular contents (light blue) and the scleral shell (dark blue). |
|
Figure 3. This graphic depicts the placement of the orbital implant into the eye socket after the patient's has been removed via either evisceration or enucleation. |
Both methods involve the placement of a spherical implant into the orbit to maintain orbital volume (Figure 3). In an evisceration, the implant is wrapped by the sclera with the extraocular muscles still attached. In an enucleation, the extraocular muscles are detached from the sclera and then attached to the implant. The tissues surrounding the eye – the tenon's capsule and conjunctiva – are then closed over the implant. Both surgeries result in the same external appearance. |
|
Figure 4. This graphic shows where the conformer sits in the eye socket. |
After the surgery, a conformer is placed into the socket as a placeholder for the future prosthesis (Figures 4 and 5). This is a large, clear, plastic shield that protects the socket and maintains its shape. It resembles a very big and thick contact lens. The conformer will need to stay in the socket for at least two months after the surgery in order to keep the pocket created by the eyelids, called the fornices, well-formed. The fornices will be the future support of the ocular prosthesis. |
|
Figure 5a. Examples of conformers. |
Figure 5b. Example of what the clear conformer looks like when it is worn in the eye socket. |
|
Figure 6. This graphic shows where the prosthetic eye sits in the eye socket. |
Once the custom prosthesis is made, usually around two months after the surgery, it will replace the conformer in the eye socket (Figures 6 and 7). |
|
Figure 7a. Example of prosthetic eyes. |
Figure 7b. Example of what the prosthetic eye looks like when it is worn in the eye socket. |
 |
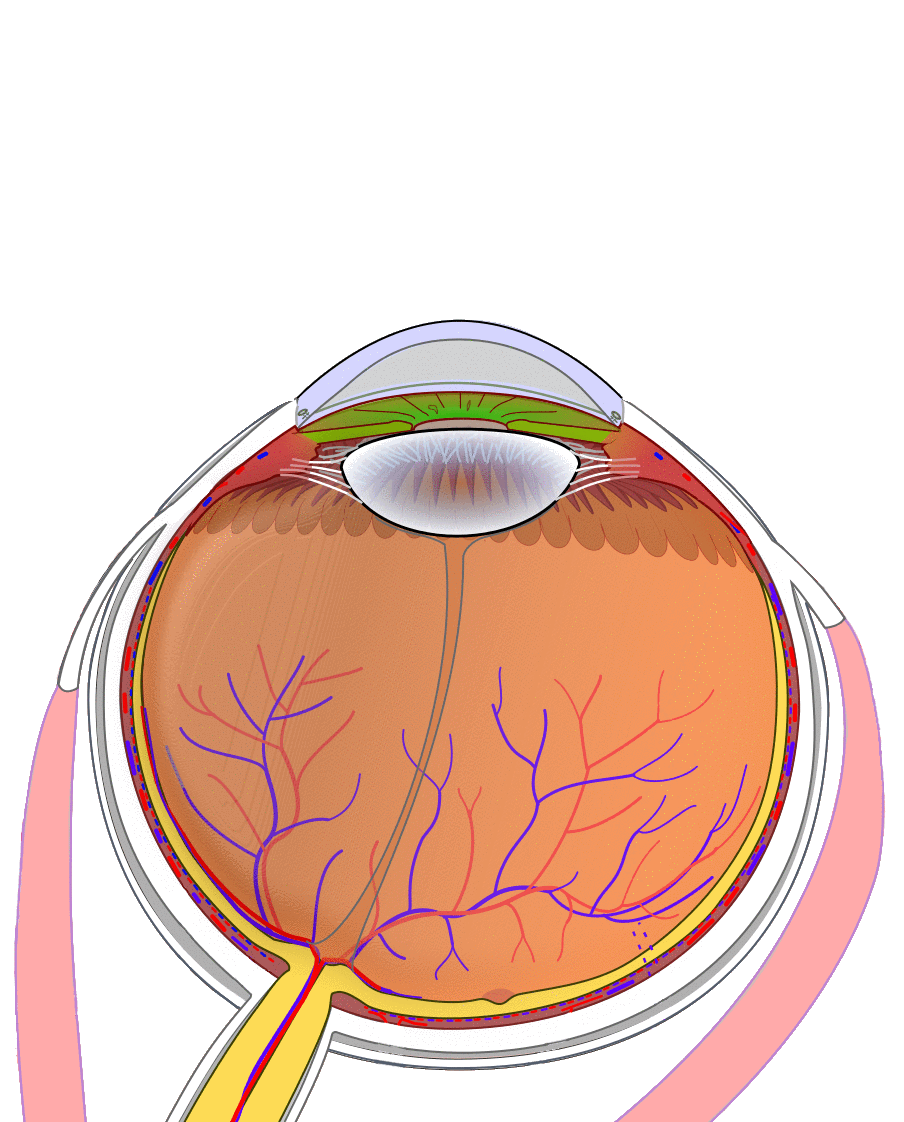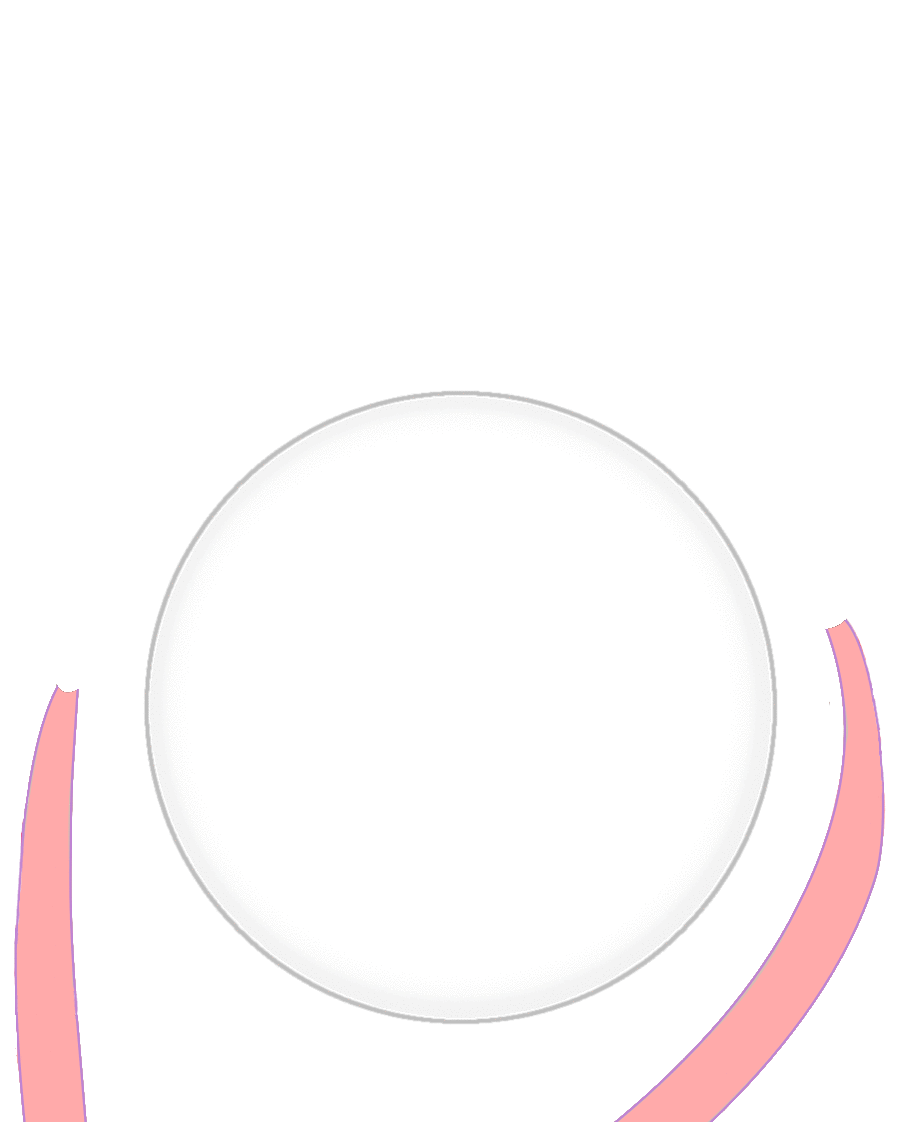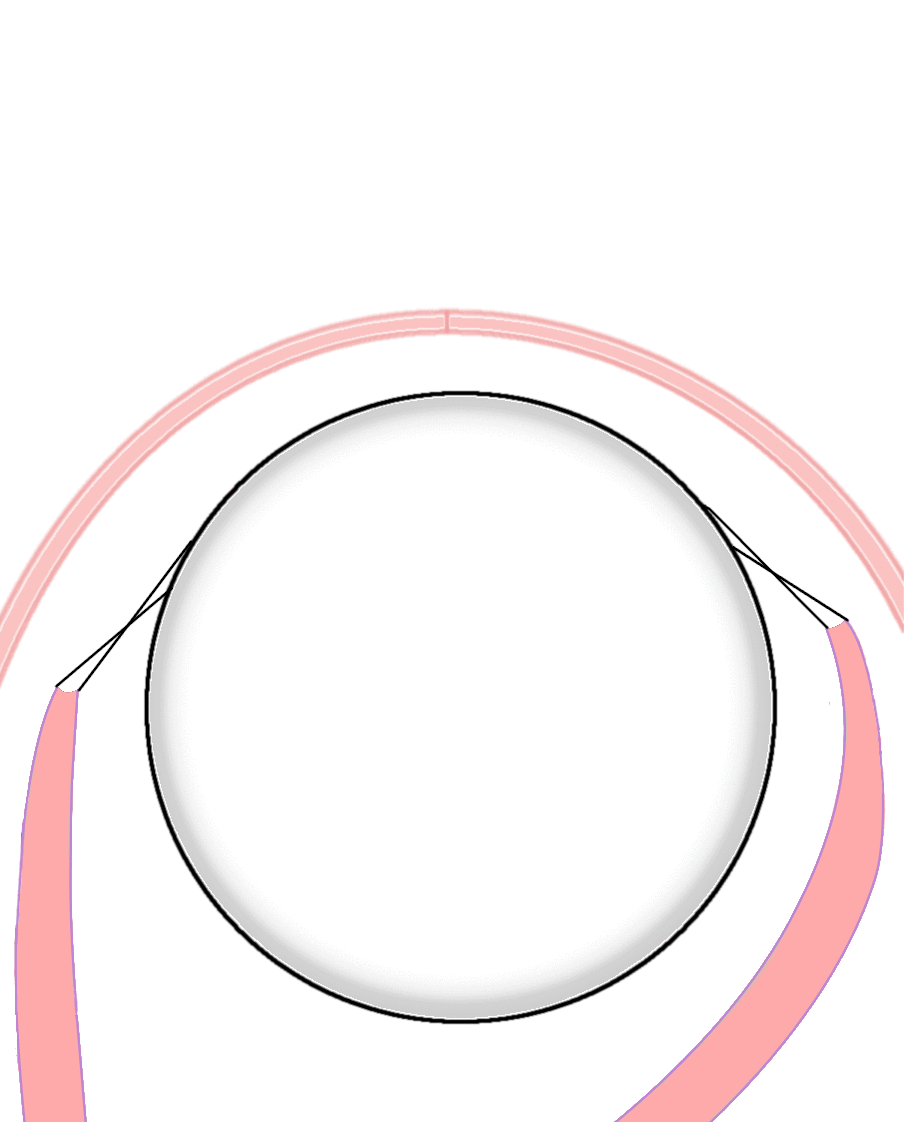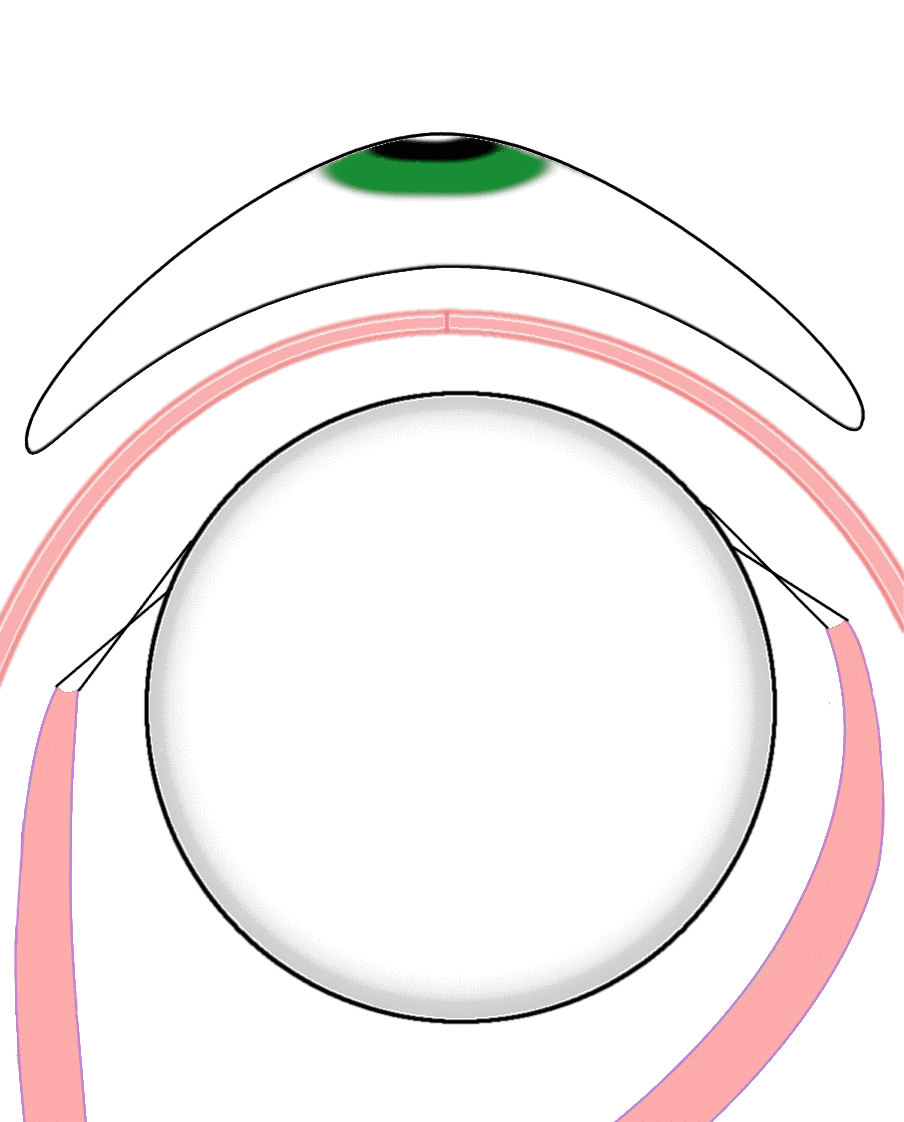 |
Figure 8. This graphic depicts the entire process of eye removal surgery, from tissue removal to prosthesis use.
Because an evisceration involves less disruption of the orbital tissues, it is a slightly shorter and simpler operation. However, depending on the reason why the eye needs to be removed, not every patient will qualify for an evisceration. Notably, cancer patients are not good candidates for an evisceration, as it will leave behind tissues that may be malignant. Additionally, enucleation is preferred in certain kinds of trauma and infection to avoid complications associated with those conditions, such as sympathetic ophthalmia.
 |
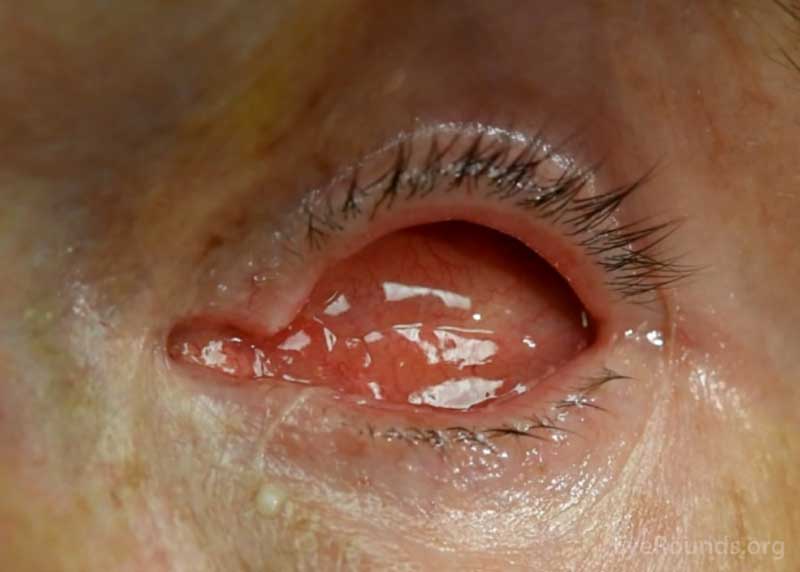 |
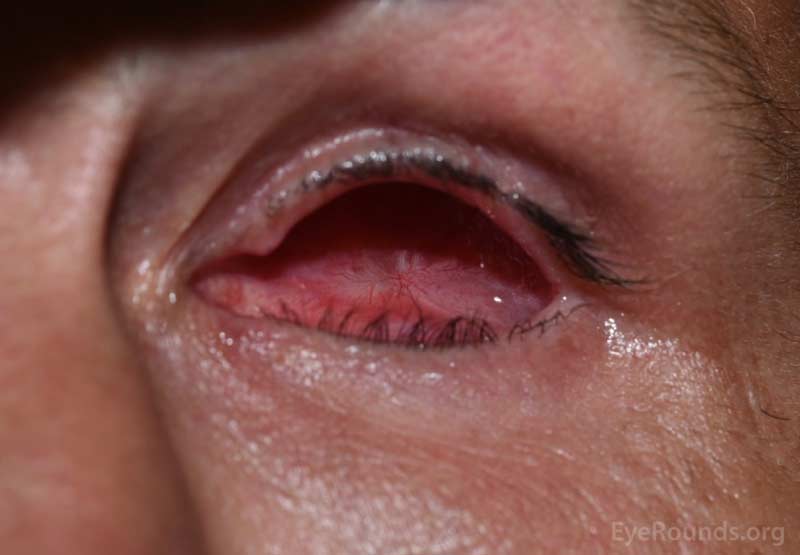
Figure 9. Examples of eye sockets after evisceration (left) and enucleation (right). Note that both sockets appear similar, regardless of the surgical technique used.
Despite the differences in technique, evisceration and enucleation have an identical external appearance afterwards, and both surgeries are effective in reducing pain and creating a suitable pocket for the insertion of a prosthetic eye, which may improve the external appearance of an unsightly eye (Figure 9).
Video 1. Demonstration of motility of an eye socket after eye removal surgery.
The motility with and without a prosthesis is also very similar between the two surgeries (Video 1).
If you are making the decision to undergo eye removal surgery, please note that both evisceration and enucleations are irreversible surgeries. It involves the removal of tissues that are not replaceable. As a result, these surgeries may rule you out as a candidate for restorative therapies that may be developed in the future.
Your preoperative consultation is important to create a plan for the eye removal surgery and determine what other medical issues need to be addressed prior to the procedure. This ensures that the surgery and anesthesia will be safe to perform.
When picking a date for your surgery, please keep in mind that you will need to avoid heavy lifting, strenuous activities, and dirty environments for at least two weeks after the surgery. You will not be able to swim for three weeks. Additionally, you will need to heal for at least 2 months before you are eligible for prosthesis fitting. Please schedule your surgery accordingly, especially if you have any upcoming events such as weddings, graduations, vacations, or work or social events.
This surgery is an outpatient surgery, which means you will go home after the surgery and will not spend the night at the hospital. You will need a driver that is 18 years or older to take you home and take care of you the night after surgery because it is not safe to drive right after the anesthesia you will be given during the procedure.
Before the surgery, you may want to find an ocularist to learn more about the process of making an ocular prosthesis. An ocularist is an artist who specializes in making artificial eyes. It may be more efficient to schedule an ocularist fitting shortly after your surgery so that you can start the insurance verification process and get your desired prosthetic made in a timely manner. The University of Iowa offers an in-house ocular prosthetics service – click here to learn more.
Eye removal surgery requires you to receive anesthesia. Depending on your other medical conditions, there are two types of sedation we may use.
For both types of anesthesia, you will have the entire area around the eye numbed for your comfort throughout the surgery. You will be awake and ready to go home shortly after the surgery.
 |
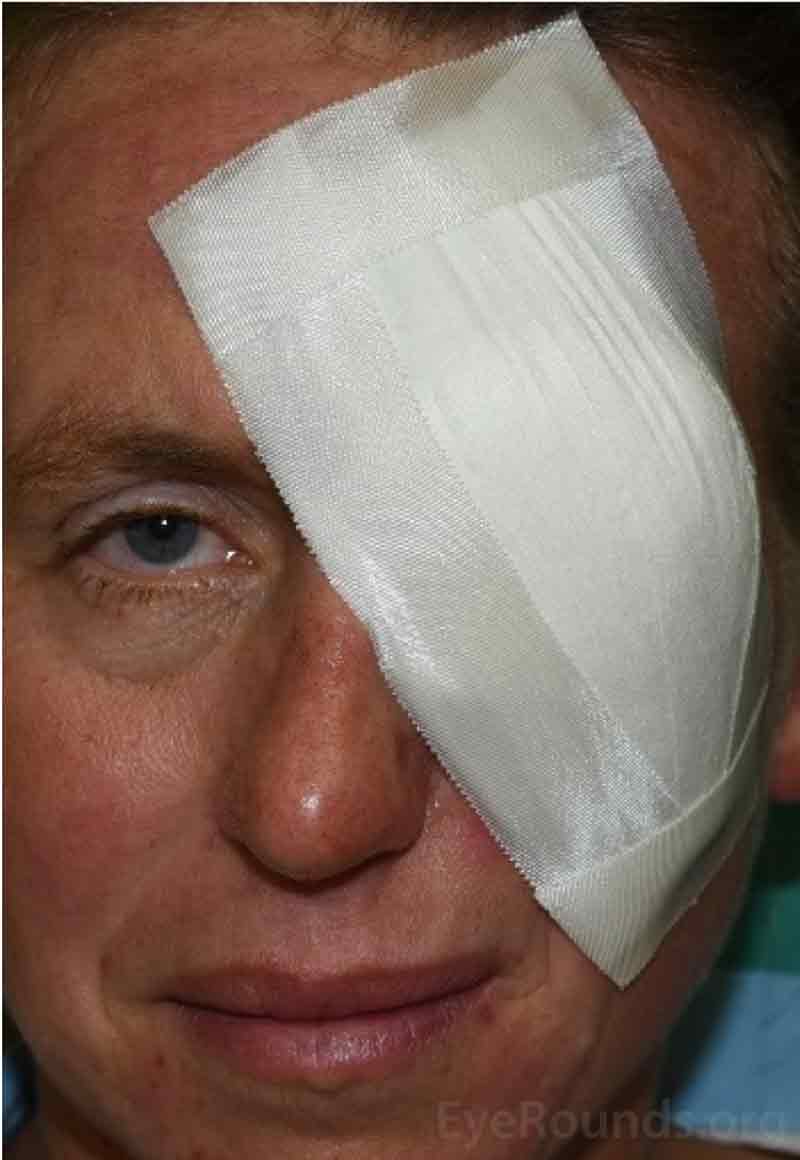 |
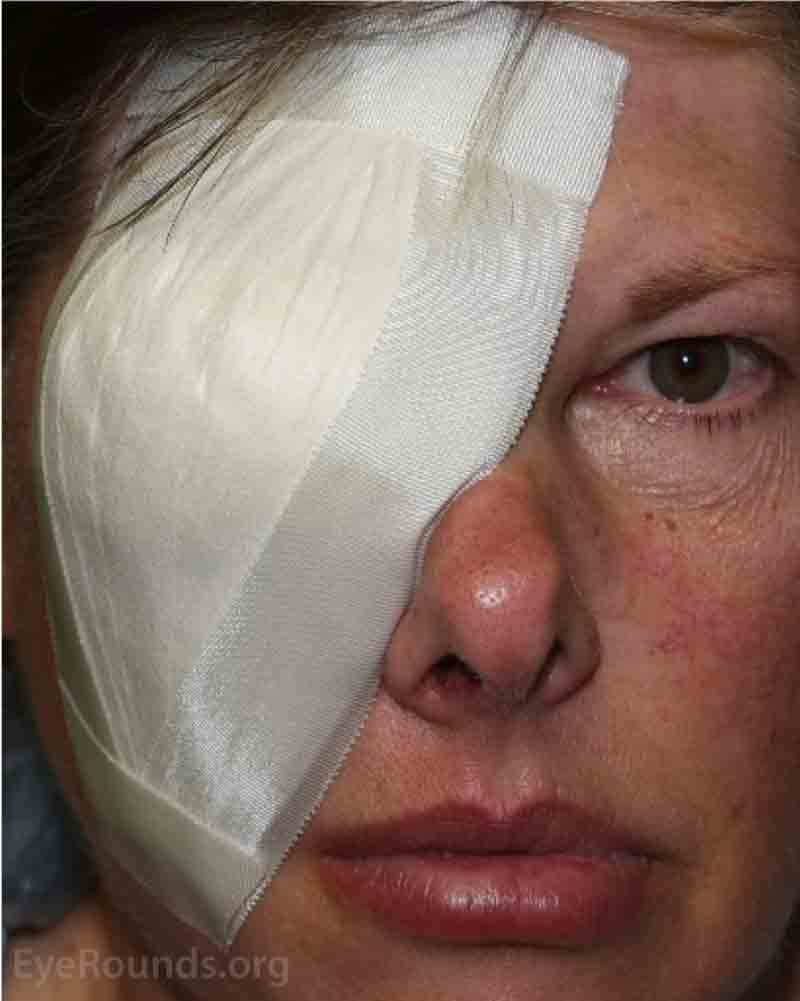
Figure 10. Examples of the patch placed over the eye immediately after the eye removal surgery.
At the end of the procedure, you will have a large pressure patch placed over the eye (Figure 10). It may be slightly uncomfortable or irritating because it will be fairly tight and may feel itchy. However, this patch is very important to keep swelling and bruising down. Do not remove the patch unless instructed otherwise. We will remove it for you at the one-week follow-up visit. You will not need to use any prescribed ointment until we take the patch off for you in the clinic. It is important that you do not get the patch wet or it will fall off.
Most patients have mild discomfort after surgery (Video 2), which comes mainly from two things:
While we do send you home with some narcotic medication, most patients do well with just acetaminophen (Tylenol). Take the pain medication as prescribed only if it is necessary.
Video 2. Patient interviews describing how the eye felt right after surgery.
Restrictions after surgery include no heavy lifting, bending at the waist, and strenuous activities for at least two weeks. Avoid dirty environments for at least two weeks after the surgery. You will not be able to swim for three weeks.
You will come back for your first follow-up visit approximately one week after surgery. At this visit, we will remove the patch for you and check for signs of healing and infection.
 |
 |
 |
|
 |
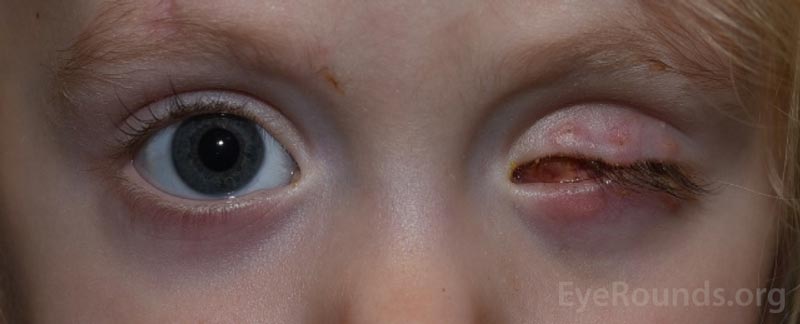 |
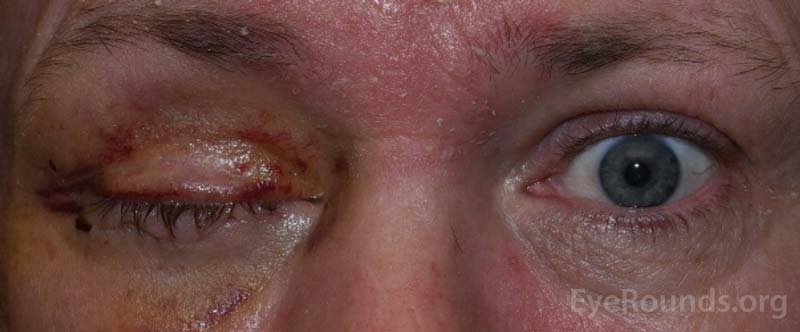
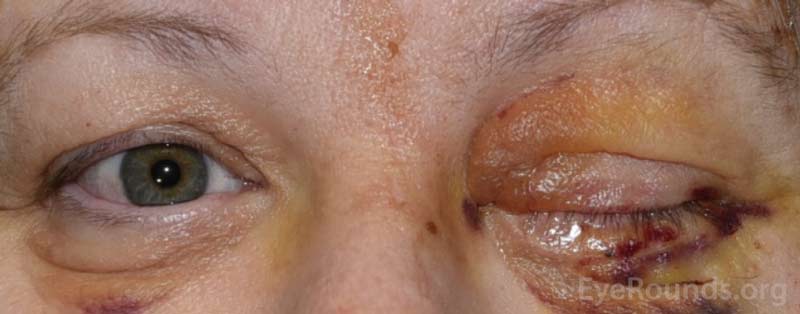
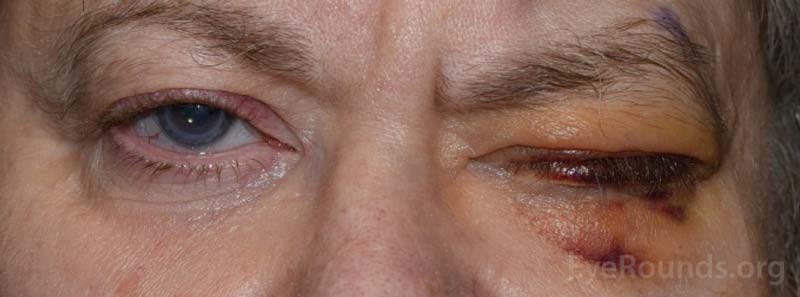
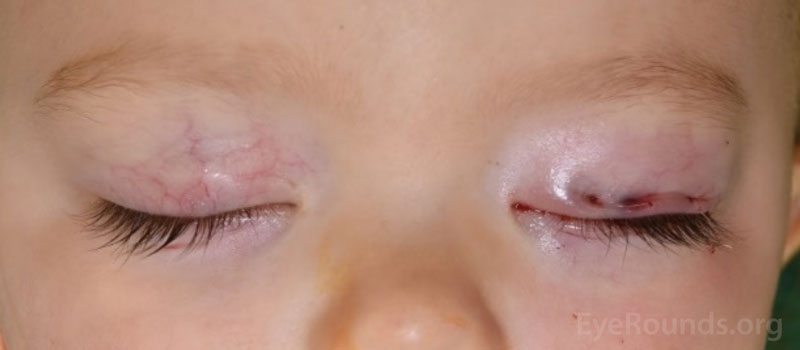
Figure 11. Examples of the bruising and swelling that is typical after eye removal surgery. Note that patients often have their eyelid temporarily sewn shut to promote healing.
After the patch is removed, you will typically see some mild swelling and bruising, which will get better over the next couple of weeks (Figure 11). Note that the eyelid may be temporarily closed. After eye removal, the eyelid is sometimes sewn shut temporarily to promote healing and keep the conformer in place. This part of the procedure is called a tarsorrhaphy. The stitches keeping the eyelid closed are dissolvable, and the eyelid will open by itself in approximately one week.
Figure 12. Example of patient wearing a conformer after their eye removal surgeries, as well as an example of what the conformer looks like.
When the eyelids open, you will see the clear conformer in place in the eye socket (Figure 12). The pink tissue behind the clear conformer is similar to the mucosal tissue on the inside of your mouth. As we discussed previously, the conformer is important for optimal healing after surgery. Its job is to protect the eye socket and maintain its shape. It needs to stay in place until your prosthesis is fitted. If the conformer falls out, you or a caregiver can put it back in just like a contact lens (Video 3). If you are unable to put it back in, please call us and we can put it back in for you (Video 4).
Video 3. Demonstration of a conformer being inserted by oneself.
Video 4. Demonstration of a conformer being inserted by another person.
Figure 13. Examples of droopiness seen after the eye removal surgery, which is often corrected after a properly fitted prosthetic eye is worn (top). If the eye continues to be droopy, eyelid adjustment surgery can address the issue (bottom).
Please note that the eyelid may seem droopy for the first few months while you are wearing the conformer (Figure 13). This is because removing the eye decreases the total volume in the orbit. The lid will often rise again once your custom fitted prosthesis is put into the socket, making up the remainder of the orbital volume. If the lid is still droopy after you are fully healed and your prosthesis is in place, we can elect to raise the lid with surgery later. The orbital volume can also be augmented with additional orbital implants or by fat grafting.
At the first week follow-up appointment, please remember to let us know which ocularist you would like to meet with for your prosthesis fitting. Patients typically schedule their two month follow-up appointment on the same day as the ocularist visit, so that right after your socket has been checked and approved by the surgeon for healing, you can start the process of being fit for a prosthesis. This will also allow us to send the necessary paperwork to get the insurance authorization started for your ocular prosthesis.
If everything is healing as we expect, your second follow-up visit will be around two months after the surgery.
 |
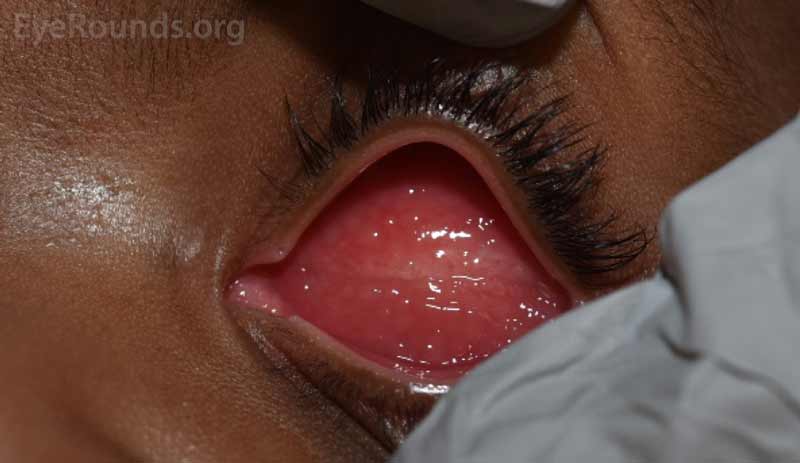 |
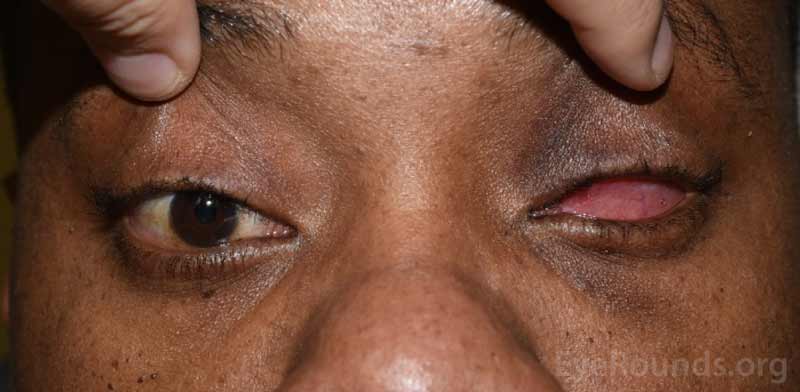
Figure 14. Example of a fully healed eye socket with (left) and without (right) the conformer in place.
After two months, the socket is well healed (Figure 14). As you can see, a pink color can be seen through the plastic conformer. Removal of the conformer reveals healthy pink mucosal tissue and well-formed pockets by the eyelids.
At this two month follow-up after your surgery, once you are approved by your surgeon to be completely healed, you may have your custom prosthetic eye made. This process usually takes two days and involves taking making a mold of your eye socket, adjusting the fit, and painting the prosthesis to match your other eye. You can learn more about making artificial eyes at the UIHC Ocular Prosthetic Service website. The clear conformer is then replaced by the prosthetic eye, which you may wear full time (Figure 15, Video 5).
Video 5. Demonstration of the insertion of a prosthetic eye. The indicator symbol (in this example, the red dot), should be facing up. To insert the prosthesis, gently lift the upper eyelid and slide the top of the prosthetic into the pocket formed by the eyelid. Then, while holding the prosthetic in place, gently pull the lower lid down over the bottom of the prosthesis. The prosthesis is secured in position in the socket by the eyelids.
Figure 15. Examples of patients wearing prosthetic eyes.
 |
 |
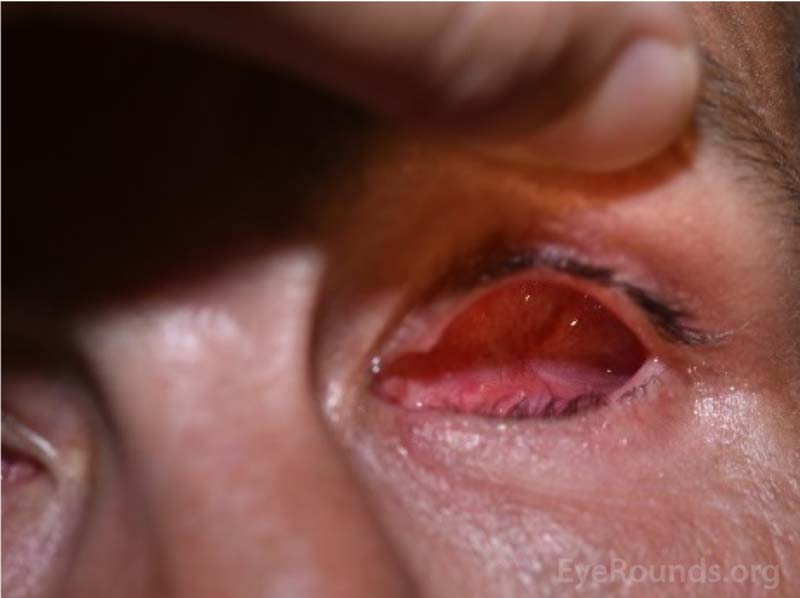
Figure 16. Examples of a socket check (left) and prosthesis polishing (right).
Your next follow-up visit will be about 6 months after surgery. Patients typically schedule a visit with the ocularist at the same time as this visit. You will need the socket checked and your prosthesis polished. Patients without an eye are recommended to have a socket check and prosthesis polish every 6 – 12 months for the rest of their lives (Figure 16).
Whether or not you take out your prosthesis between visits is your personal choice. Some patients leave the prosthesis in and only have the doctor and ocularist remove it during their checkups. Other patients are comfortable removing it and putting it back in, and even choose to clean it regularly using baby shampoo. Regardless, it is very important to regularly get your prosthesis polished by your ocularist, as this will remove scratches, mineral and protein buildups, and harmful bacteria from the surface of the prosthesis. This leads to a healthier socket and a more natural appearance to the artificial eye. Some patients do experience dryness while wearing their prosthesis, which can be irritating and cause difficulty blinking. If this happens, there are a variety of lubricants that may help alleviate any discomfort. Many patients recommend mineral oil as their lubricant of choice, as it works very well and is cost effective. It is usually applied directly onto the prosthesis once in the morning and once at night, but you can adjust this schedule however you like. Other lubricants that are commonly used include artificial tears, eye gels, and lubricating eye drops. Anything that can be used in the seeing eye can be used with your prosthesis. Your ocularist will be able to recommend the best lubricant for your specific needs.
Because the prosthesis can be a choking hazard, many parents recommend discouraging younger children from removing the prosthesis at all. Additionally, consider insuring the prosthesis under your homeowner's policy in case the prosthesis is lost.
Additional precautions need to be taken in patients with only one eye, as it becomes even more important to protect the remaining vision in that eye. It is vital that you establish care with a regular eye care provider for annual dilated eye exams in addition to seeing your oculoplastic surgeon annually. Let your regular eye care provider know immediately if you see any flashes of light, floaters, or experience decreased vision in your remaining eye.
 |
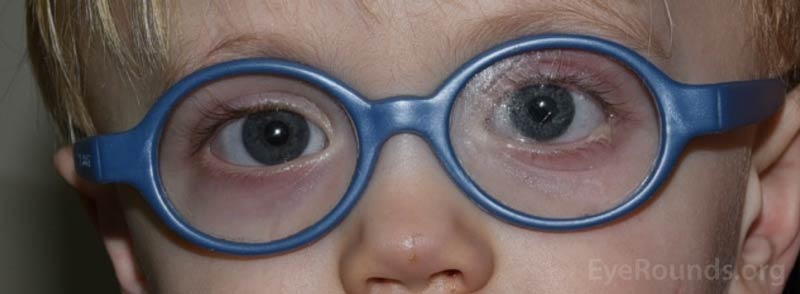 |
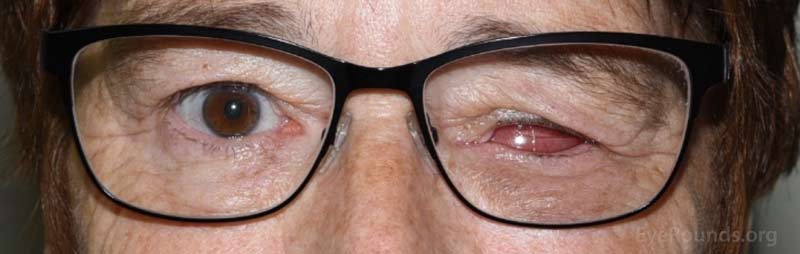
Figure 17. Examples of patients wearing protective polycarbonate lenses.
To protect your seeing eye against any trauma or accidents, please wear polycarbonate lenses. If possible, we recommend that you do not engage in high risk activities and employment (Figure 17).
Whether because of trauma, cancer, or a variety of other eye diseases, patients who have had an eye removed overwhelmingly report improved self-confidence, pain relief, and an increased ability to function in their daily lives (Videos 6 and 7). Prosthetic eyes nowadays are very lifelike, and it is often very hard to tell that someone has had an eye removed at all. Some patients even choose to have fun with their prosthesis, adding fun designs or hidden images (Figure 20).
Video 6. Advice to parents of young children who are having an eye removed.
Video 7. Patient interviews talking about the experience of eye removal surgery and life afterwards with an ocular prosthesis.
Figure 20. Examples of prosthetic eyes with unique designs.
Figure 21ab. Examples of customized prosthetic.
If you would like to learn more about your eye removal surgery and what comes after, there are many resources available, written by doctors, patients, and their caregivers. These are some of our recommendations:
Yom KH, Ricca AM, Shriver EM, Ko AC. Enucleation and Evisceration: What to Expect. EyeRounds.org. posted September 27, 2017; Available from: https://eyerounds.org/cases/279-anophthalmic-socket.htm

Ophthalmic Atlas Images by EyeRounds.org, The University of Iowa are licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License.