
Scleritis is a severe, immune-mediated ocular inflammatory condition that is frequently associated with systemic immunologic disease. The condition is classified by location (anterior or posterior) and the appearance of scleral inflammation (diffuse, nodular, or necrotizing).
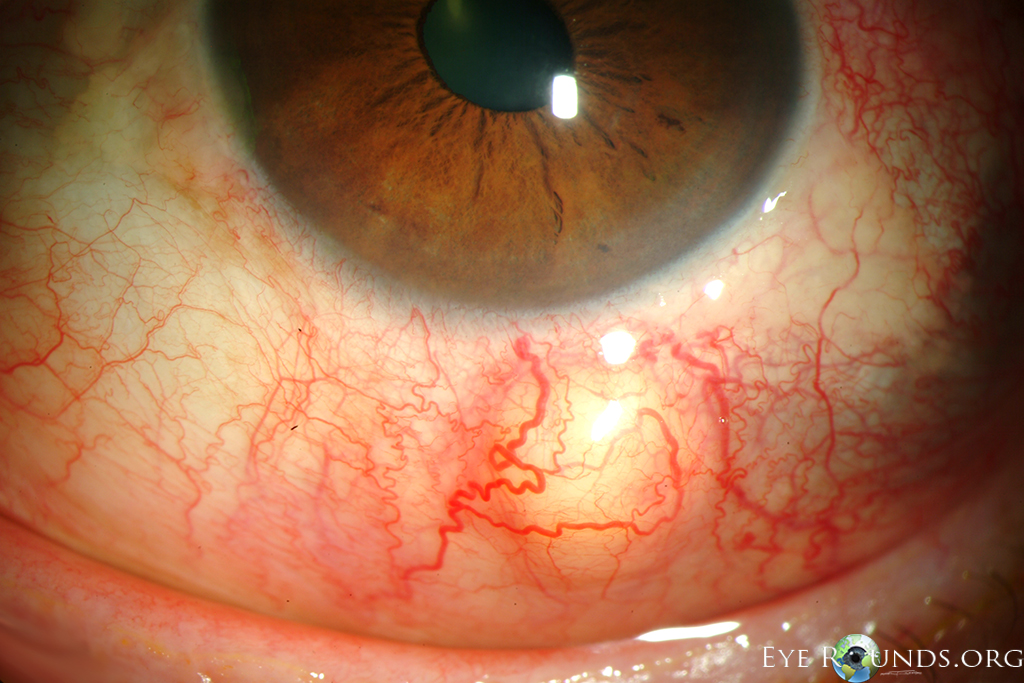
Nodular anterior scleritis: Anterior scleritis may present in diffuse, nodular, or necrotizing forms. Patients with nodular scleritis present with one or more firm, tender nodules. This image shows nodular thickening of the sclera with typical violaceous hue due to dilated scleral vessels. There is also overlying dilation of the conjunctival and episcleral vessels and mild chemosis. While conjunctival and episcleral involvement are often seen overlying active nodular scleritis, scleral involvement is necessary to make this diagnosis. Scleritis is often associated with underlying systemic autoimmune diseases such as rheumatoid arthritis, granulomatosis with polyangiitis (formerly called Wegener's granulomatosis), spondyloarthritis, or systemic lupus erythematosus. Treatment is with systemic and topical non-steroidal anti-inflammatory drugs, systemic steroids, or systemic immunosuppression. Newer literature suggests that subconjunctival steroids may be effective in non-necrotizing cases.

Ophthalmic Atlas Images by EyeRounds.org, The University of Iowa are licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License.