Thyroid Eye Disease
A Summary of Information for Patients
Chase A Liaboe, BA (M4), Brittany A. Simmons, MD*, Thomas J Clark, MD, Erin M Shriver, MD
September 1, 2016; updated January 9, 2017; *updated January 17, 2020
Introduction
Thyroid eye disease (TED) is an inflammatory disease of the eye and the surrounding tissues. The inflammation is due to an autoimmune reaction - the body's immune system is attacking tissues within and around the eye socket. TED is sometimes referred to by other names, such as Graves' ophthalmopathy, Graves' orbitopathy, thyroid-associated ophthalmopathy, and/or thyroid orbitopathy.
About 90% of TED patients also have Graves' disease, an autoimmune disorder that causes excess thyroid hormone production (hyperthyroidism). However, 10% of patients with TED have either a normal-functioning or under-functioning thyroid (e.g. Hashimoto's thyroiditis). While control of systemic thyroid hormone levels is crucial in patients with TED, the ocular disease course and severity does not always correlate with thyroid hormone levels.
Most patients with TED have signs and/or symptoms in both eyes, however the severity can differ between the eyes. Some of the most common manifestations of TED:
- Swelling in and around the eye socket
- Retraction (tightening) of the eyelids
- Strabismus (the eyes are not in alignment with each other) and diplopia (double vision)
- Dry, irritated, red eyes
More severe ocular effects from TED are rare, but can occur and include vision loss from damage to the optic nerve and breakdown/infection of the cornea (the transparent, outermost layer of the eye that we see through).
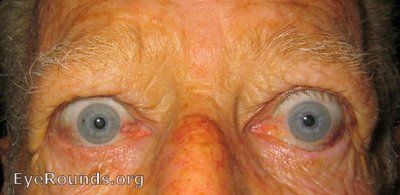 |
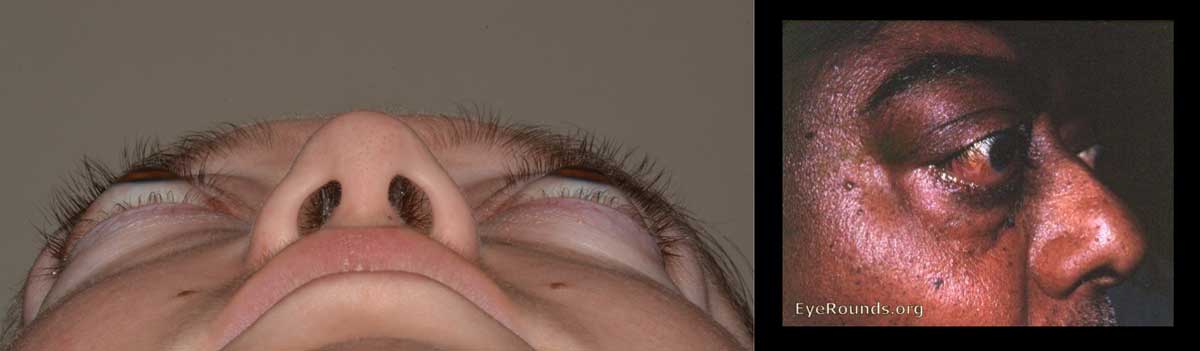
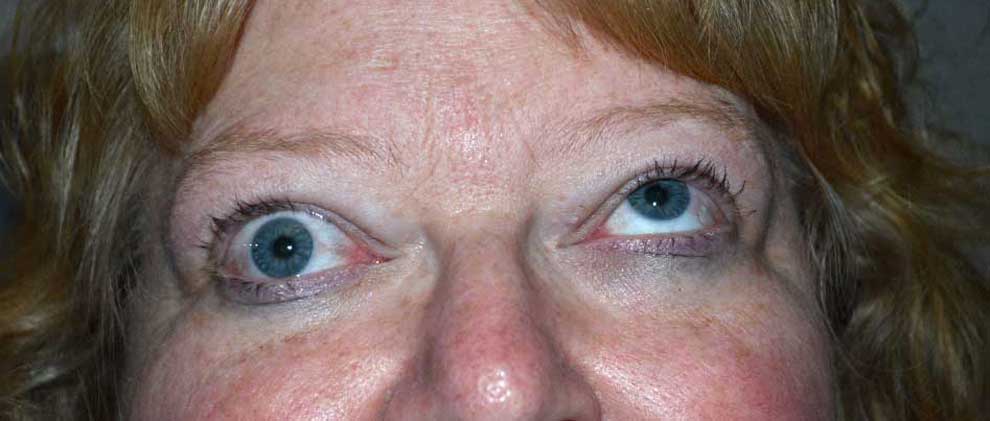
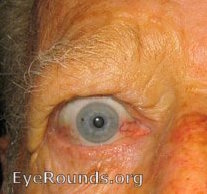
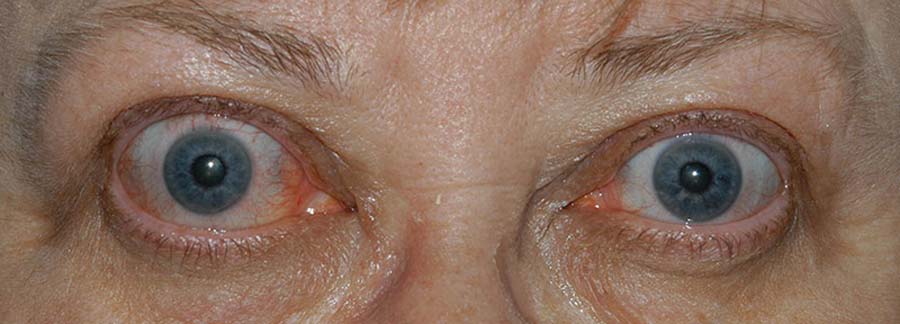 |
Figures 1 and 2. These patients have some of the classic signs and symptoms of TED. Note the swelling around the eye, retraction of the eyelid, and injection of the conjunctiva.
Epidemiology
- TED is the most common cause of both orbital disease and exophthalmos (external protrusion of the eyeball from the socket) in North America and Europe.
- TED occurs more frequently in women than in men, with both sexes having two age ranges in which TED is most likely to be diagnosed.
- Females
- 16 per 100,000 (0.016%) females have TED
- Most diagnoses occur between 40-44 and 60-65 years old
- Males
- 3 per 100,000 (0.003%) males have TED
- Most diagnoses occur between 45-49 and 65-69 years old
- Females
- Risk factors for the development of TED include the following
- Age (see above age ranges)
- Sex (females more likely to be diagnosed with TED)
- Ethnicity (higher incidence among people of black and Asian/Pacific Island ethnicity) [1]
- Family history of TED or other thyroid disorders
- Smoking, or exposure to tobacco smoke
- Thyroid dysfunction (particularly hyperthyroid) [2]
- Presence of thyroid stimulating hormone receptor antibodies/thyroid stimulating immunoglobulin [3]
- Radioactive iodine therapy [4]
- The signs, symptoms, and severity of TED can be worsened by both genetic and environmental factors.
- Smoking or exposure to cigarette smoke
- Smokers are twice as likely to develop Graves' disease
- Smokers with Graves' disease are over 7x more likely to develop TED, when compared to nonsmokers
- Smokers tend to have a longer duration of the active phase of TED (2-3 years for smokers, compared to 1 year for nonsmokers)
- Selenium deficiency [5] (see Selenium)
- Vitamin D deficiency [6]
- Increased stress levels (see Stress reduction)
- Smoking or exposure to cigarette smoke
Mechanism of TED
TED is caused by an inflammatory response involving the tissues in and around the eye socket.
- TED patients produce autoantibodies (proteins of the immune system that aberrantly react against the body's own cells) that bind to fibroblast cells within the eye socket
- When these antibodies bind, they cause the fibroblast cells to produce and release chemical signals and biologic materials that lead to swelling and congestion in and around the eye socket
- The main autoantibody produced by TED patients is known as Thyroid Stimulating Immunoglobulin (TSI), and this autoantibody can be measured in the blood to help monitor disease activity
- The amount of TSI present in a TED patient correlates with TED severity
- However, sometimes TED can occur without TSI formation
Clinical Presentation of TED
About 90% of patients with TED also have some thyroid dysfunction - usually the thyroid is overactive (i.e. Graves' disease), but occasionally the thyroid is underactive (e.g. Hashimoto's thyroiditis). Most times, the diagnosis of TED and diagnosis of a thyroid dysfunction occur within the same year. Patients who are diagnosed with TED but have no known thyroid dysfunction should see their primary care physician for an evaluation of their thyroid function.
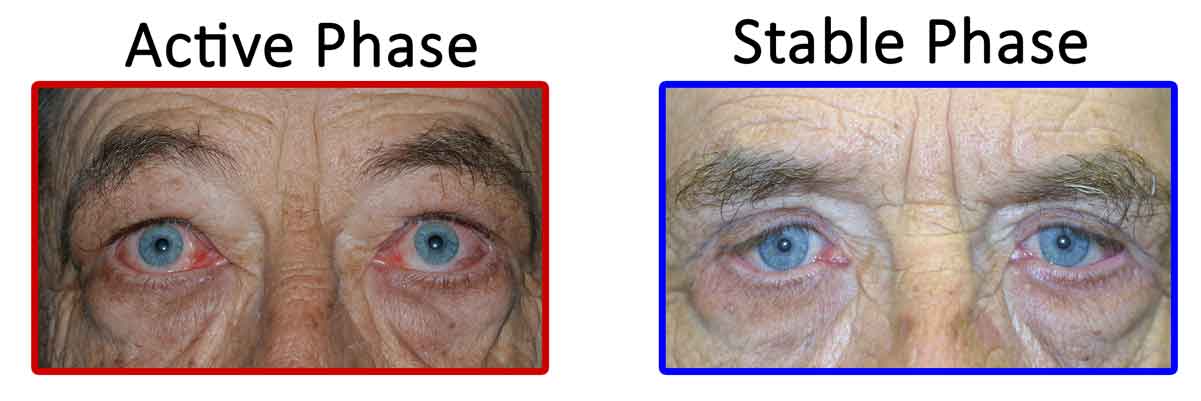
The disease course for TED involves 2 phases - active and stable. In the active phase there is active swelling and inflammation. This presents as redness in and around the eye, eye pain with or without eye movement, as well as swelling around the eyes and eyelids. The active phase of TED involves a waxing/waning period of these symptoms, and can last months to years. On average, the active phase of TED lasts about 1 year for non-smokers, and 2-3 years for smokers (or patients exposed to smoke). The active phase of TED spontaneously transitions to the stable phase, but can recur. Active TED has a recurrence rate of about 5-10%, but is less likely to recur after 18 months in the stable phase.
Figure 3. Active vs. Stable TED. Active TED is characterized by signs of inflammation (swelling around the eye, swelling and injection of the conjunctiva, and enlargement of the muscles that move the eye). TED activity waxes and wanes, and usually transitions to stable TED within 1-3 years.
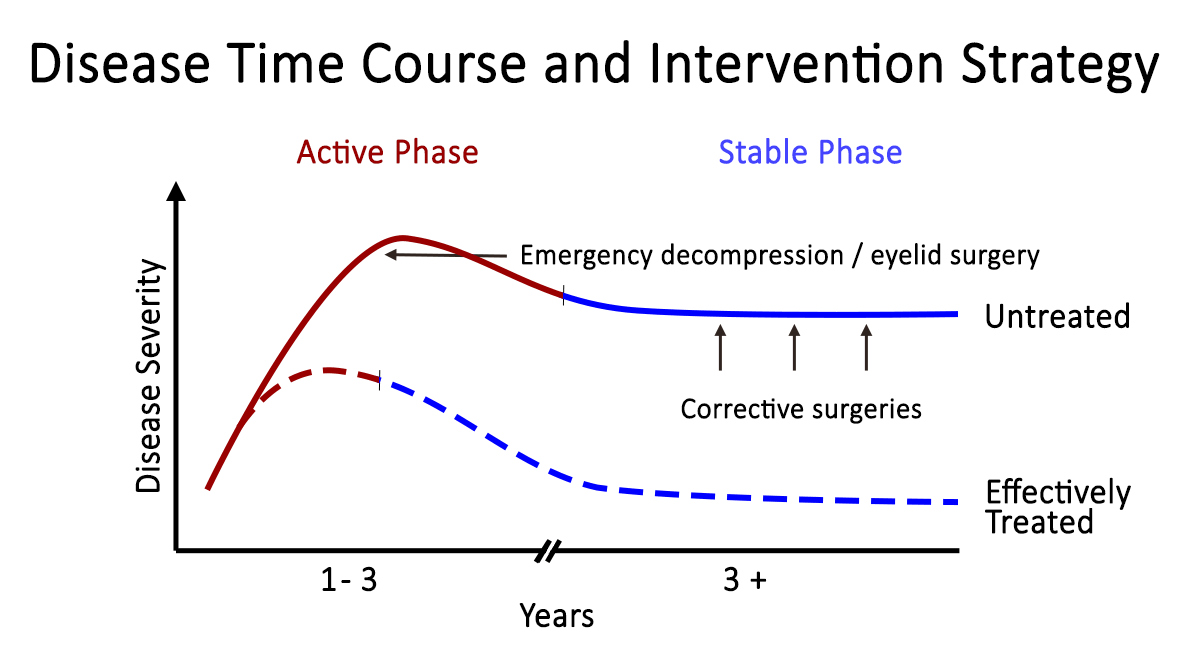
Figure 4. Rundle's curve. As seen in the representation of TED activity over time in Rundle's curve, initiating therapy early is crucial to diminish the overall severity of the chronic disease.
Many patients with TED present to a physician with similar complaints. The most common signs and symptoms associated with TED are
- Upper and/or lower eyelid retraction - the eyelid is pulled away from its normal resting position
- Affects up to 90% of TED patients, and can affect one or both eyes
- On exam, there is a larger palpebral fissure (the space between the upper and lower eyelids) and the eyes have a characteristic "startled/surprised" appearance
- In cases of severe retraction, it may become difficult to close the eyelids at rest, leading to dry eyes, which can lead to tearing, foreign body sensation, and blurred vision
- It is important to treat dry eyes, starting with liberal use of preservative-free eye drops, in addition to eye ointment at night
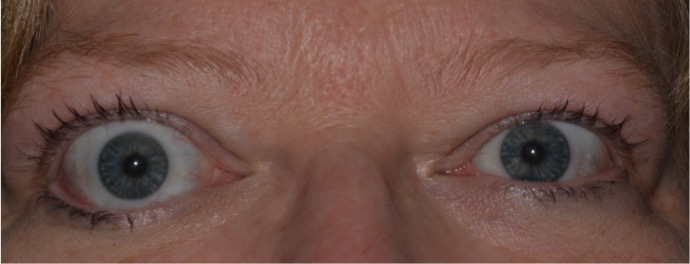
Figure 5. Eyelid retraction is the most common presenting sign of TED, and is the result of many factors associated with TED.
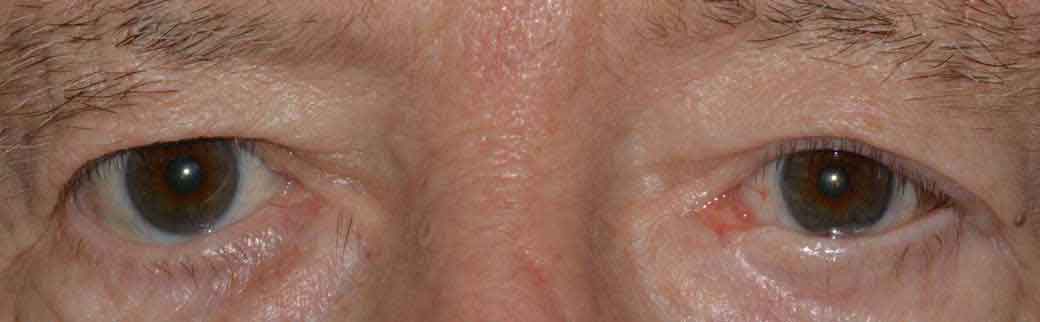
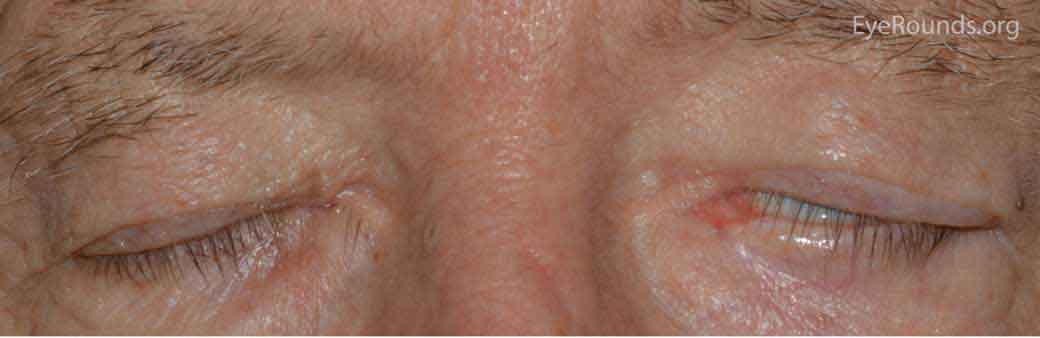
Figure 6. Lagophthalmos is the inability of the eyelid to fully close. It typically presents as dry eye, tearing, foreign body sensation, and blurred vision.
Figure 7. Temporal flare. Note the elevation of the outer portion of the normal eyelid.
- Exophthalmos/Proptosis - bulging of the eyeball out of the eye socket
- Affects up to 60% of TED patients
- Most commonly leads to dry eye and excessive tearing
- It is important to treat dry eyes, starting with liberal use of preservative-free eye drops, in addition to eye ointment at night
- In severe cases, damage to the cornea can result
- This can be treated with the dry eye therapy listed above in addition to decreasing the palpebral fissure (distance between the upper and lower eyelids) with surgery to close the outer and/or inner corners of the eyelids (tarsorrhaphy), lowering the upper lid, raising the lower lid, or orbital decompression surgery (See Below)
- In rare cases, proptosis can cause globe subluxation, which is a displacement of the eye out of the eye socket
- This is an eye emergency, and needs to be addressed immediately
Figure 8. Exophthalmos, also known as "proptosis," is when the eyeball is displaced out of the eye socket. This is an eye emergency – the cornea is at risk of drying out, and the optic nerve is at risk of irreversible damage.
- Restrictive extraocular myopathy - swelling of the muscles that control eye movement resulting in inadequate mobility of the eyes
- Affects up to 40% of TED patients
- One or both eyes are restricted in how far they are able to move
- In more severe instances, the eye muscles can be affected at rest leading to misalignment of the eyes
- This can cause strabismus (i.e. "crossed eyes"), which is a cause of diplopia (double vision).
- Permanent correction of restrictive myopathy is not typically performed until the patient has been in the stable phase of TED for several months.
- Temporary correction can be undertaken with adding prism lenses to the patient's glasses
- When the patient has been in the stable phase of TED for several (typically at least 6) months, surgical correction of strabismus can be considered
- Pain with eye movement
- Affects about 30% of TED patients
- Characterized as a dull, deep orbital pain
- Can usually be managed with over-the-counter NSAIDs
- Optic nerve dysfunction / compressive optic neuropathy
- Affects about 6% of TED patients
- The eye is encased in a confined, bony eye socket. With progressive inflammation and swelling of the muscles and tissues surrounding the eye, the pressure within the eye socket can increase, leading to damage of the optic nerve
- Warning signs include
- Decrease or change in color vision
- Decreased peripheral vision
- Decreased crispness of central vision
- Warning signs include
- This is an eye emergency, and needs to be addressed urgently by an ophthalmologist
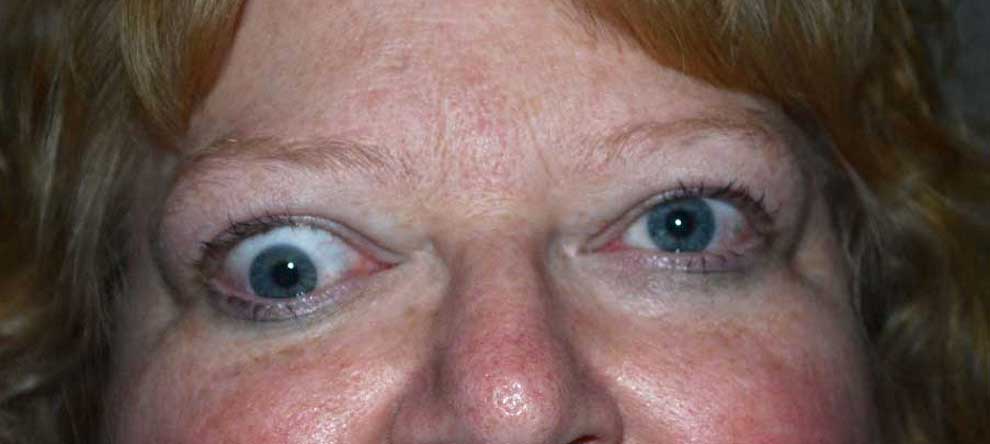
Figure 9. Hypotropia is when an eye is deviated downwards in comparison to the other eye, when looking straight ahead. This misalignment is due to an enlarged and restricted orbital muscle.
Figure 10. Esotropia is when an eye is deviated inward in comparison to the other eye, when looking straight ahead. This misalignment is due to an enlarged and restricted orbital muscle.
Figure 11. Chemosis is swelling within the conjunctiva.
Figure 12. Conjunctival injection is caused by the dilation of the vessels within the conjunctiva. (larger image not available)
Evaluating the Activity and Severity of TED
When examining patients with TED, it is important to document both the current activity and severity of disease. This helps both the patient and physician track the course of the disease as well as monitor for signs and symptoms of "flare-ups" or disease recurrence. In addition, management is based on both the activity and severity of disease, making proper disease categorization of great importance in determining proper treatment strategies.
To assess the activity level of TED, the Clinical Activity Score (CAS) can be used
- At the initial visit, patients are given a CAS score of 1-7 (one point for each of the following signs or symptoms)
- Spontaneous pain in or around the eye in the past 4 weeks (pain without eye movement)
- Eye pain associated with eye movement in the past 4 weeks
- Swelling of the eyelids
- Redness of eyelids
- Conjunctival injection (redness of the actual eyeball)
- Chemosis (swelling of the eyeball)
- Swelling of the caruncle (the red prominence at the inner corner of the eye)
Initial Visit (1 point each)
CAS ≥ 3 → "Active" |
Follow-up Visit (1 point each)- Criteria 1-7
CAS ≥ 4 → "Active"
|
- At subsequent follow-up visits, the 3 following criteria are added for a potential CAS score of 10
- Increase in proptosis/exophthalmos (bulging of the eye out of the eye socket) of the eye (by at least 2mm)
- Decrease in motility of an eye in one direction (by at least 8º)
- Decrease in vision (by at least 1 line on the Snellen chart)
- TED is considered "active" if the CAS ≥ 3 at the initial visit, or ≥ 4 at follow-up visits
To grade the severity of TED, many indices are used, two of which are mentioned below
- NOSPECS
- Class 0: No signs or symptoms
- Class 1: Only signs (upper lid retraction)
- Class 2: Soft tissue involvement (swelling of the eye or tissues surrounding the eye)
- Class 3: Proptosis (bulging of the eye out of the eye socket)
- Class 4: Extraocular muscle involvement (usually with strabismus)
- Class 5: Corneal involvement (severe dry eye from inability to adequately close the eye)
- Class 6: Sight loss (due to optic nerve involvement)
- The European Group of Graves' Orbitopathy (EUGOGO) classifies TED severity into three categories
- Mild
- Only a mild impact on daily life
- Insufficient signs/symptoms to justify immunosuppressive drugs or surgical treatment
- One or more of the following
- Minor lid retraction (<2mm)
- Mild soft tissue involvement
- Proptosis (bulging of the eye out of the eye socket) <3mm above normal for race and gender
- Transient or no diplopia (double vision)
- Dry eye symptoms responsive to lubricants/ointments
- Moderate-to-severe
- Non sight-threatening, but has sufficient impact on daily life to justify immunosuppression or surgical intervention
- One or more of the following
- Lid retraction ≥ 2mm
- Moderate or severe soft tissue involvement
- Exophthalmos ≥ above normal for race and gender
- Transient or constant diplopia
- Sight-threatening
- TED patients with optic neuropathy and/or corneal breakdown
- Warrants immediate intervention
- Mild
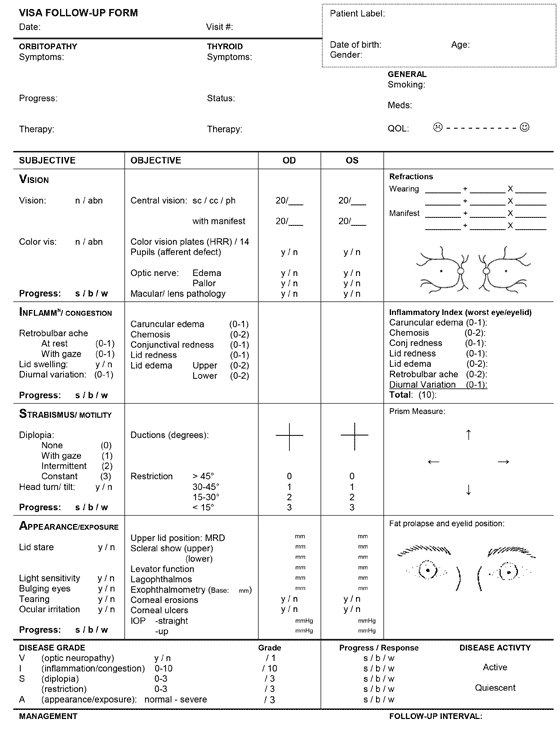
Finally, both activity and severity of TED can be assessed with the VISA analysis, which evaluates Vision, Inflammation, Strabismus, and Appearance. (SEE VISA CHART)
Figure 14. VISA chart
Treatment
First and foremost, patients with TED should maintain good general health and well-being. Research suggests optimizing selenium and vitamin D levels may be beneficial. In addition, it is important to achieve normal systemic thyroid hormone levels, especially in patients who undergo thyroid treatment (e.g. radioactive iodine ablation, thyroidectomy, etc.) Smoking cessation is extremely important in TED patients - it will help maintain stable thyroid hormone levels, as well as decrease the duration of the active phase of the disease. As previously mentioned, smokers are twice as likely to develop Graves' disease and 7x more likely to develop TED compared to nonsmokers. Additionally, smoking reduces the effectiveness of many treatments used for TED.
It is important to initiate treatment for TED at the time of diagnosis in order to decrease the final severity of the disease. Early initiation of treatment has been shown to be most effective at decreasing the final severity of the disease. Early intervention during the active phase allows for correction of inflammation and swelling within the eye and its surrounding tissues, which decreases the degree of permanent tissue scarring.
The majority of patients with TED have mild to moderate disease, and require mostly "supportive care" including- Dry eye management with preservative-free drops and ointments (topical cyclosporine can be added if symptoms persist)
- Lifestyle modifications such as:
- Smoking cessation
- Sodium restriction (reduces water retention in the tissues surrounding the eyes)
- Sleeping with the head of the bed elevated (to decrease swelling around the eyes)
- Sunglasses (decreases dryness and helps with light sensitivity)
- Mineral supplementation with Selenium (taken regularly) has been shown to significantly benefit patients with mild TED in Europe (see Selenium)
- Oral NSAIDs for eye pain
- Prism lenses (may be used long term or as a temporary measure until surgical correction can be considered) for patients with strabismus (misalignment of the eyes)
- Selenium
- When taken regularly for one year, selenium has been shown to exert significant benefits in patients with mild, non-inflammatory orbitopathy in Europe where the soil is selenium deficient
- The benefits of selenium supplementation from non-selenium-deficient populations is not known
- Stress reduction
- Recently, studies have been conducted to evaluate the role of stress in patients with thyroid disorders, including TED.
- Specific hormones are released in response to stress, and these hormones affect thyroid hormone levels, thus impacting TED.
- While the current research is not strongly evidenced-based and mostly circumstantial, many clinical studies have observed an association of stress and the severity (or recurrence)of TED.
- Recently, studies have been conducted to evaluate the role of stress in patients with thyroid disorders, including TED.
Figure 15. Rundle's curve. As seen in the representation of TED activity over time in Rundle's curve, initiating therapy early is crucial to diminish the overall severity of the chronic disease.
Medical Treatment Options, A brief overview
Again, it is important to optimize thyroid function for a euthyroid state, and this is often achieved through medications like methimazole or propylthiouracil for hyperthyroid states, and levothyroxine for hypothyroid states. Please realize that each TED patient has a unique presentation, requiring different treatment regimens.
- Corticosteroid Therapy
- Steroids have many beneficial properties in treating TED
- They prevent and reduce inflammation, leading to decreased swelling of tissue in and around the eyes
- They down-regulate the immune system, which limits TED (an autoimmune disease)
- However, many patients do not respond completely (or at all) to steroid treatment, and some patients have their symptoms recur when weaning off or discontinuing the steroids.
- Treatment with oral steroids (e.g. prednisone) is most common
- Patients typically start with a high dose, and then slowly taper over the course of several months
- The overall mean effectiveness rate for oral steroids is about 60%
- Drawbacks and side effects include
- Partial response, or no response at all
- Relapse of signs/symptoms with tapering or discontinuing therapy
- Cushing syndrome
- Weight gain
- Increased risk of infection
- Worsening of diabetes, hypertension (high blood pressure), and osteoporosis
- Treatment with high-dose intravenous (IV) steroids has been shown to be more effective (about 70% success rate) than oral steroids, however this form of therapy requires weekly clinic visits
- Treatment usually lasts 12 weeks, with treatment administered once per week
- With high-dose IV steroids, there is greater risk for toxicity but this decreases with lower IV doses
- Frequent monitoring of electrolytes, liver function, and blood pressure is required
- A low risk of liver toxicity, electrolyte disturbances, and arrhythmias exists.
- Steroids have many beneficial properties in treating TED
- Biologic Immunomodulators
Glucocorticoids have traditionally been first line therapy for the treatment of thyroid eye disease. The treatment of thyroid eye disease is currently undergoing a paradigm shift and some physicians have advocated for initial treatment with biologic therapies. These treatments target different molecules or pathways believed to be involved in thyroid eye disease.
- Mycophenolate mofetil reduces proliferation of B and T cells of the immune system and also suppresses antibody formation by B cells. A recent randomized, masked, multicenter trial of 164 patients showed patients treated with steroids followed by a prolonged course of mycophenolate (83 patients) had statistically significant improvement in symptoms, eyelid swelling, and caruncle swelling compared to patients treated with steroids alone (81 patients) [7]. A separate single center study comparing 80 patients treated with mycophenolate versus 78 patients receiving steroid treatment showed statistically significant improvement in diplopia, as well as an average ≥3mm reduction in proptosis in the patients treated with mycophenolate. While there was disease reactivation in some patients treated with steroids, there was no disease reactivation in the mycophenolate group [8]. In both studies, more patients responded to treatment with mycophenolate, and duration of response was longer with mycophenolate compared to steroids.
- Tocilizumab blocks the immune signaling receptor for interleukin-6 (IL-6) and may reduce disease activity [9]. A prospective study of 18 patients resistant to previous steroid treatment found significant improvement in ocular disease symptoms as well as diplopia. There was also improvement in proptosis, though this was not significant [10]. A subsequent small randomized, controlled multicenter study of tocilizumab treatment in 15 patients who had failed steroid therapy demonstrated a statistically significant reduction in ocular symptoms compared to 17 patients treated with placebo, with improvement in both diplopia and proptosis that did not reach statistical significance [11].
- Rituximab depletes B cells of the immune system. Studies yield conflicting results. A randomized trial of 31 patients treated with rituximab (15 patients) versus steroids (16 patients) demonstrated a statistically significant reduction in symptoms and improvement in ocular motility in the rituximab group. The steroid group exhibited a similar ability to significantly reduce ocular symptoms, though there was disease reactivation and need for more surgical intervention compared to the rituximab group [12]. Similar results were seen in a separate study, where 9 patients were treated with rituximab. Compared to 20 patients treated with steroids, the rituximab group demonstrated a significant reduction in proptosis and inflammation, improvement in symptoms and no disease recurrence [13]. However, a small randomized study of 21 patients, 11 treated with rituximab compared to 10 with placebo, showed no significant reduction in symptoms, diplopia, eyelid position, or proptosis [14].
- Infliximab, adalimumab, and etanercept block Tumor Necrosis Factor (TNF), an immune signaling molecule. Data is limited, with only a handful of studies typically of 10 patients or fewer; however, etanercept has been associated with statistically significant reduction in symptoms, as has adalimumab in severely inflamed patients [15,16]. Of note, approximately 30% of the patients treated with etanercept experienced disease reactivation. Few case reports exist for infliximab therapy, and this currently appears to be a potential treatment option for patients with severe thyroid eye disease who have failed steroids and decompression surgery [17].
- Teprotumumab is an antibody that targets a key molecule involved in thyroid eye disease, insulin-like growth factor-1 receptor (IGF-1R). Clinical trials have been promising. A randomized, controlled, multicenter trial of 42 patients treated with teprotumumab showed approximately 70% of patients with active, moderate to severe thyroid eye disease had a statistically significant decrease in symptoms and a meaningful reduction in proptosis of ≥2mm. This is in comparison to 45 patients treated with placebo, with only 20% of placebo-treated patients seeing similar improvement in symptoms and at least a 2mm reduction in proptosis [18,19]. This medication was recently approved in January 2020 for the treatment of thyroid eye disease.
Many of these biologic immunomodulators have shown promising results, and other biologic agents are currently under investigation; however, current data is derived from relatively few studies with a small number of patients. Additional randomized prospective trials, with an increased number of patients and longer follow up, are needed.
- Orbital Radiotherapy (ORT)
- ORT is commonly used in conjunction with corticosteroids
- ORT works by decreasing the autoimmune response of TED, as well as preventing the congestion and swelling of tissue in and around the eye socket, including the extraocular muscles responsible for moving the eye
- ORT reduces the amount of inflammation in TED patients, especially with patients who have experienced compressive optic nerve damage, tissue inflammation around the eye, and restrictive extraocular myopathy
- Risks associated with ORT
- Increased inflammation initially post treatment
- Increased incidence of retinal damage
- Patients with diabetic and/or hypertensive retinopathy are at an increased risk of retinal damage
- Increased risk of cataract formation
- Theoretical risk of causing a secondary cancer
- A recent small study of phosphorus-based plaque radiation therapy showed promise in reducing proptosis and thyroid eye symptoms without significant short-term side effects [20]. Radiation side effects can show up years later, however, so further studies are needed to determine the long-term efficacy and consequences of localized plaque radiation.
- Compared to corticosteroids or ORT monotherapy, a combination of ORT with corticosteroids has a more sustained anti-inflammatory effect, leading to a decreased risk of compressive optic neuropathy in active TED [21].
About 20% of patients with TED require some sort of surgical intervention, with 13% undergoing eyelid surgery, 9% undergoing strabismus surgery, and 7% undergoing orbital decompression (for compressive optic nerve damage and/or proptosis).
Most surgical intervention occurs after the patient has been in the stable phase of TED for at least 6 months, with the exception of urgent orbital decompression for compressive optic neuropathy or eyelid surgery such as a tarsorrhaphy for exposure keratopathy (destruction of the cornea due to severe dry eye). By waiting for disease stability, the treating physician is reassured that the disease is unlikely to recur and that the signs and symptoms are unlikely to progress further. In general, surgery is not advised while the patient's thyroid is dysfunctional - thus it is important to attain normal thyroid hormone levels during the initial management.- Orbital Decompression Surgery
- Occasionally required if excess pressure on the optic nerve leads to vision loss that is rapidly progressive
- The procedure relieves pressure (on the optic nerve and blood supply) in the eye socket by removing bone, allowing excess tissue to expand/decompress from the confined bony socket.
- There are many different approaches to orbital decompression surgery and different parts of the eye socket can be decompressed.
- Correction of Strabismus
- TED can cause swelling and tightening of the muscles that control eye movements (restrictive extraocular myopathy), leading to strabismus (crossed eyes), and diplopia (double vision)
- Most TED patients with diplopia do not require surgical intervention, but can be managed with prism lenses until the disease enters the stable phase
- If diplopia persists in the stable phase, or if strabismus leads to abnormal head positioning, surgery can be considered
- Surgery involves repositioning the muscles that control eye movement
- For patients who were unable to be treated with prism lenses, and are poor surgical candidates, botulinum toxin (i.e. Botox™) injections into the extraocular muscles can be considered.
- Correction of Eyelid Retraction
- There are both surgical and non-surgical approaches to treating eyelid retraction
- Non-surgical approaches may be best suited for patients who are in the active phase of the disease experiencing evolving eyelid changes, those not interested in surgery, or for patients who are poor surgical candidates bothered by the cosmetic effects of thyroid eye disease. In these cases, injectable therapies may offer a temporary solution.
- Steroid injection may improve eyelid position in the early stages of thyroid eye disease by reducing active inflammation that leads to fibrosis of the eyelid muscles. [22]
- Fillers commonly used to restore facial volume and minimize wrinkles can be injected to promote extension of the eyelid via mass effect. [23]
- Botulinum toxin (i.e. Botox™) can be injected into the muscles that control the eyelid, helping them relax and lower from their retracted position. [24]
- There are many surgical approaches available to correct eyelid retraction
- The muscles that control the eyelids can be surgically altered to relieve tension of the eyelids (e.g. a "blepharotomy" is a surgical procedure in which the eyelid is cut in order to help lengthen the eyelid from its retracted position)
- Eyelid "weights" or spacer material (i.e. ear cartilage, hard palate from the mouth, sclera, or synthetic material) can be implanted into the upper eyelid to help the eyelid descend from its retracted position.
References
- McLeod DS, Caturegli P, Cooper DS, Matos PG, Hutfless S. Variation in rates of autoimmune thyroid disease by race/ethnicity in US military personnel. JAMA 2014;311:1563-5. [PMID 24737370]
- Prummel MF, Wiersinga WM, Mourits MP, Koornneef L, Berghout A, van der Gaag R. Effect of abnormal thyroid function on the severity of Graves' ophthalmopathy. Arch Intern Med 1990;150:1098-101. [PMID 1691908]
- Diana T, Kahaly GJ. Thyroid stimulating hormone receptor antibodies in thyroid eye disease-methodology and clinical applications. Ophthalmic Plast Reconstr Surg 2018;34:S13-9. [PMID 29771755]
- Stan MN, Bahn RS. Risk factors for development or deterioration of Graves ophthalmopathy. Thyroid 2010;20:777-83. [PMID 20578901]
- Khong JJ, Goldstein RF, Sanders KM, et al. Serum selenium status in Graves' disease with and without orbitopathy: a case-control study. Clin Endocrinol (Oxf) 2014;80:905-10. [PMID 24372054]
- Heisel CJ, Riddering AL, Andrews CA, Kahana A. Serum vitamin D deficiency is an independent risk factor for thyroid eye disease. Ophthalmic Plast Reconstr Surg 2020;36:17-20. [PMID 31568022]
- Kahaly GJ, Riedl M, König J, et al. Mycophenolate plus methylprednisolone versus methylprednisolone alone in active, moderate-to-severe Graves' orbitopathy (MINGO): a randomised, observer-masked, multicentre trial. Lancet Diabets Endocrinol 2018;6:287-98. [PMID 29396246]
- Ye X, Bo X, Cui H, Lu B, Shao J, Wang J. Efficacy and safety of mycophenolate mofetil in patients with active moderate-to-severe Graves' orbitopathy. Clin Endocrinol (Oxf) 2017;86:247-55. [PMID 27484048]
- Leszczynska A, Molins B, Fernandez E, Adan A, Ortiz-Perez S. Cytokine production in thyroid eye disease: in vitro effects of dexamethasone and IL-6 blockade with tocilizumab. Graefes Arch Clin Exp Ophthalmol 2019;257:2307-14. [PMID 31338585]
- Perez-Moreiras JV, Alvarez-Lopez A, Gomez EC. Treatment of active corticosteroid-resistant graves' orbitopathy. Ophthalmic Plast Reconstr Surg 2014;30:162-7. [PMID 24503568]
- Perez-Moreiras JV, Gomez-Reino JJ, Maneiro JR, et al. Efficacy of tocilizumab in patients with moderate-to-severe corticosteroid-resistant Graves orbitopathy: a randomized clinical trial. Am J Ophthalmol 2018;195:181-90. [PMID 30081019]
- Salvi M, Vannucchi G, Curro N, et al. Efficacy of B-cell targeted therapy with rituximab in patients with active moderate to severe Graves' orbitopathy: a randomized controlled study. J Clin Endocrinol Metab 2015;100:422-31. [PMID 25494967]
- Salvi M, Vannucchi G, Camp I, et al. Treatment of Graves' disease and associated ophthalmopathy with the anti-CD20 monoclonal antibody rituximab: an open study. Eur J Endocrinol 2007;156:33-40. [PMID 17218723]
- Stan MN, Garrity JA, Carranza Leon BG, Prabin T, Bradley EA, Bahn RS. Randomized controlled trial of rituximab in patients with Graves' orbitopathy. J Clin Endocrinol Metab 2015;100:432-41. [PMID 25343233]
- Paridaens D, van den Bosch WA, van der Loos TL, Krenning EP, van Hagen PM. The effect of etanercept on Graves' ophthalmopathy: a pilot study. Eye (Lond) 2005;19:1286-9. [PMID 15550932]
- Ayabe R, Rootman DB, Hwang CJ, Ben-Artzi A, Goldberg R. Adalimumab as steroid-sparing treatment of inflammatory-stage thyroid eye disease. Ophthalmic Plast Reconstr Surg 2014;30:415-9. [PMID 24978425]
- Durrani OM, Reuser TQ, Murray PI. Infliximab: a novel treatment for sight-threatening thyroid-associated ophthalmopathy. Orbit 2005;24:117-9. [PMID 16191800]
- Smith TJ, Kahaly GJ, Ezra DG, et al. Teprotumumab for thyroid-associated ophthalmopathy. N Engl J Med 2017;376:1748-61. [PMID 28467880]
- Douglas RS. Teprotumumab, an insulin-like growth factor-1 receptor antagonist antibody, in the treatment of active thyroid eye disease: a focus on proptosis. Eye (Lond) 2019;33:183-90. [PMID 30575804]
- Hao HT, Wang Y, Wang X, et al. Treatment of Graves' ophthalmopathy with an in-house phosphorus-32 source: initial clinical observations. Exp Ther Med 2017;14:2795-800. [PMID 28966670]
- Rajendram R, Bunce C, Lee RW, Morley AM. Orbital radiotherapy for adult thyroid eye disease. Cochrane Database Syst Rev 2012;11:CD007114. [PMID 22786503]
- Xu D, Liu Y, Xu H, Li H. Repeated triamcinolone acetonide injection in the treatment of upper-lid retraction in patients with thyroid-associated ophthalmopathy. Can J Ophthalmol 2012;47:34-41. [PMID 22333849]
- Zamani M, Thyagarajan S, Olver JM. Functional use of hyaluronic acid gel in lower eyelid retraction. Arch Ophthalmol 2008;126:1157-9. [PMID 18695117]
- Costa PG, Saraiva FP, Pereira IC, Monteiro ML, Matayoshi S. Comparative study of Botox injection treatment for upper eyelid retraction with 6-month follow-up in patients with thyroid eye disease in the congestive or fibrotic stage. Eye (Lond) 2009;23:767-73.
Suggested Citation Format
Liaboe CA, Simmons BA, Clark TJ, Shriver EM. Thyroid Eye Disease: A Summary of Information for Patients. EyeRounds.org. March 4, 2020; Available from: http://eyerounds.org/patients/thyroid-eye-disease.htm